Vaginoplasty Revisions
Welcome to Legacy Surgical Partners – we look forward to caring for you! Our priority is to make your surgery process and everything in between as pleasurable, empowering, and accessible as possible. Patients are expected to follow guidelines established by the WPATH Standards of care Version 8. We follow these standards—not as a gatekeeping hurdle—but as minimal guidelines that are useful guideposts that are protective. Though regret for gender affirming surgery is extremely rare, we are medical professionals who are here at your bequest. Surgery is irreversible, which puts the onus of responsibility on both patient and provider.
We're here to help you make essential decisions and know what to expect in surgery planning and recovery. Our team consists of:
- Surgeons
- A physician assistant
- Medical assistants
- Our surgery scheduler
- Office team
- And you
That's right, you! We value your input, your perspective and all the work you are and will be doing to prepare for and recover from surgery. We look forward to getting to know you better and learning how we can help you.
We want to make your surgery and recovery as smooth as possible. We’ll answer any questions you have and make sure you have the best possible outcome.
I. Vaginoplasty Revisions Overview
We know this surgery is extremely important. It takes incredible trust to allow a surgeon to perform this operation. We want you to know we are humbled by that trust and take it very seriously.
The first step in this process is understanding your options and creating a plan that meets your needs. We’ve created this overview to help you make important decisions and know what to expect.
What is genital feminizing revision surgery?
After your previous genital feminizing procedure, you may be looking for revision to improve functionality and/or aesthetics. Typically, our surgeries are done in one stage with historical revisions necessary approximately 10% of the time. When revision is necessary, it is important to determine if the concerns are aesthetic, functional or both. Revisions on other surgeons present unique problems but are creatively addressed while attempting to preserve aspects of the previous surgical result that are desirable. Our goal is not to pass judgment on a former surgeon but to add or improve upon what you have while minimizing scarring. Typical goals of revision surgery include:
- External improvement in symmetry, fat distribution, labial definition, clitoral hood, clitoris size and location. Urethral spraying or misdirection may also be addressed.
- Internal improvements such as destruction of retained hairs or granulation tissue or removal of excessive scar tissue.
- Canal deepening or reopening after depth is lost.
Each patient’s surgery plan and results are different.
II. Before Surgery
Before your first consultation, we encourage you to:
- Consider your goals and priorities of surgery. Consider potential complications and aspects of revision that may not necessarily be crucial to your self-image.
- Write down your questions and bring them with you to your visit.
- You may ask a support person to come with you, as two are often able to enhance the experience with deeper questioning and recollection of details
Your First Consultation
Your first consultation is an opportunity for us to learn about your hopes and goal. Your surgeon will review various surgical options and explain the process. Once we understand your goals, we will:
- Evaluate your anatomy.
- Pre-operative pictures may be taken.
- Assess your overall health to see which surgeries can meet your goals.
A fair amount of time is spent during the consultation with your surgeon. In addition, you will likely meet the other members of your care team.
Genital Feminizing Revision Options
There are many techniques available and the terminology used could differ from office to office. We will cover the most common techniques used for revision. We will go over which options are ideal for you and which techniques can be combined to achieve your surgical objectives during your appointment.
Labiaplasty
Labiaplasty may be performed as a planned second-stage procedure following traditional two-stage vaginoplasty techniques used by non-Legacy surgeons, or as part of a revision after gender-affirming vaginoplasty performed by Bowers/Gunther (approximately 10%) or by other surgeons. Our team has extensive experience with the full spectrum of surgical techniques, having revised vaginoplasty procedures from across the United States and around the world.
The goal of this procedure is to correct, rebalance or enhance surgical definition of the inner labia (labia minora). If the outer labia (labia majora) need revision, it is usually done via fat transfer, fat grafting or scar revision.
Ideal Candidate:
Anyone with previous vaginoplasty seeking improved cosmetics of the vulva, regardless where their primary surgery was performed.
Surgical Approach:
Local tissues are mobilized or modified surgically to enhance labial definition or symmetry. It is our goal to utilize existing scars and not create new ones. Local fat is often mobilized from beneath the mons skin or labial skin to fill areas of depression whose effect is to add youthfulness to the tissues. Skin flaps or mattress suturing techniques are selectively utilized where appropriate.
Limitations:
Care delivered outside Legacy Partners can be particularly challenging and is more difficult to correct–though we find it a welcome challenge in terms of creativity and artistry. Adequate tissue is necessary to form labia though this challenge can typically be performed by mobilizing local tissue or use of local skin flaps.
Fat Transfer/Fat Grafting
Local fat from under the skin or mons area often presents as an exterior bulge after GAV but can be rotated as a vascularized flap to fill skin or surface deficits. Occasionally, traditional liposuction and fat grafting can be performed where indicated.
Ideal Candidate:
Anyone with previous GAV seeking improved cosmetics of the vulva, regardless where their primary surgery was performed.
Surgical Approach:
No new scars are used for fat transfer. With fat grafting, a small amount of fat is taken from another part of the body–most commonly the abdomen–and injected into the labia majora to give more fullness and balance.
Limitations:
Depends on individual fat content and occasionally local scarring that limits ideal external contour. In fat grafting, there is also a moderate amount of fat atrophy.
Scar Revision
Widened, thick or irregular scars are unacceptable as outcomes in primary vaginoplasty. While we remain averse to such an outcome, we seek improved aesthetics, particularly on this measure–both in our patients and from those whose primary surgery is performed elsewhere. Keloid scarring, while common in less vascularized parts of the body–such as the back or chest–is not usually a problem in vaginoplasty. Healing from revision surgery is usually much quicker, typically less than 2 weeks off work and 4 weeks in recovery.
Ideal Candidate:
Individuals who are at least 6-12 months out from their primary vaginoplasty, allowing sufficient time for tissue maturation, resolution of postoperative swelling, and scar stabilization, and who have residual asymmetry or thickened scarring.
Surgical Approach:
We ask the body to do incredible healing after primary vaginoplasty. A second procedure refreshes the old scars and allows the surgeon to reapproximate the skin edges with less tension and less reactive suture material, generally resulting in scars that are straighter and more likely to fade. Occasionally, localized injection of anti-inflammatory medication can help to reduce reactivity and scarring.
Limitations:
Everyone's healing is individualized. Given proper healing we expect improvement in scar quality and appearance the degree of improvement will be different from person to person.
Hoodplasty
A clitoris that is too exposed or too covered can warrant surgical revision. Hoodplasty addresses this uncommon problem to expose the more buried clitoris or more commonly to cover the overly exposed clitoris.
Ideal Candidate:
Anyone at least 6-12 months out from primary vaginoplasty with an exposed or buried clitoris.
Surgical Approach:
A 2-layer closure is used to close local skin though it typically results in a small vertical scar above the clitoris. If the clitoris is buried, it is mobilized, anchored and exposed.
Limitations:
While in most cases we achieve the ideal amount of coverage some can be left with some residual over exposure or buried position of the clitoris
Erectile Tissue Removal
During primary vaginoplasty, much of the erectile tissue is removed; however, some is always left behind as this tissue is needed for arousal and to maintain blood supply to some portions of the healing tissues. In healing, some of the erectile tissue can shift inferiorly, allowing it to be a visible or functional problem, particularly during arousal. Occasionally, this tissue can physically block vaginal entry. Removing this tissue allows for return of function.
Ideal Candidate:
Anyone at least 6-12 months out from primary vaginoplasty with excess erectile tissue in the front portion of the vagina or along the labia minora.
Surgical Approach:
In this procedure, previous scars are utilized which allows access to the areas to be excised. This is normally planned and often marked with your surgeon.
Limitations:
Because erectile tissue is highly vascular and prone to bleeding, vasoconstrictive medication is used during surgery to minimize blood loss. As the medication wears off, patients may experience more postoperative swelling or bruising in this area compared with other aspects of revision surgery. Despite the importance of this tissue in sexual arousal, sensation is typically not significantly affected.
Urethroplasty
This procedure involves shortening, lowering, or redirecting the urethra when the urinary stream is positioned too far forward. We strongly encourage patience following vaginoplasty, as tissue maturation, reduction in swelling, and softening of scars take time. It is surprising how often minor urinary spray issues resolve with full healing over approximately six months. In some cases, excess volume of the labia majora may cross the midline and deflect the urinary stream, which can be an indication for labiaplasty. In others, a small amount of residual erectile tissue may contribute and benefit from selective removal. By repositioning the urethra into a more anatomically female location, urinary stream direction can be significantly improved in most patients.
Ideal Candidate:
Anyone at least 6-12 months out from primary vaginoplasty with urine stream abnormalities.
Surgical Approach:
The urethra is lowered or tissue is removed–erectile tissue or inner labial skin–to divert the urine stream to the desired central position. Scars are very similar to the scars before surgery. A foley is usually placed over the weekend and removed in a clinic visit.
Limitations:
Delicate surgical technique and judgment are necessary for a good result. We expect improvement in nearly all patients however degree of improvement can vary from patient to patient and can take several months to realize final results.
Vaginal Reopening Procedure (VRP)
Loss of depth has multiple causes though the most common cause of vaginal stenosis (medical term for narrowing or closure of the vagina) is failure to dilate. We say ‘failure’, not in judgment but to admonish those of you who cannot or will not make the time to dilate to please maintain what you have. Dilation, unfortunately, is a daily ritual (at least for the first 18 months) that must be maintained.
If you find yourself losing depth, please seek medical advice—this can be through our office, surgeon or PA or through your PCP back home. Occasionally, pelvic floor therapy can be a useful adjunct in working with you to attain and maintain suitable depth. Sometimes, the problem can be scar tissue, pain, bleeding or granulation tissue that makes it difficult or discouraging to dilate. When you do seek evaluation, bring your dilators.
Regardless of the cause, vaginal stenosis can be a real problem. Before considering VRP,VDP, or RPFV, ask yourself why the loss of depth occurred initially and, if regained, what will you do differently? Do you need the vagina re-opened for sexual purposes or for your own sense of identity? Are you sexually active now or are you just hoping to expand your hypothetical options? Can you be faithful to a rigorous dilation schedule if depth is regained? Could you be ok with minimal depth if it means no further dilation routines and am still able to function sexually with my partner?
The process of VRP is accomplished by re-opening the apex of the vagina along the original scar lines and/or treating scar or granulation tissue.
Ideal Candidate:
Suitable candidates at least 9-12 months out from primary vaginoplasty with complete or partial closure of the vaginal canal, typically due to issues with dilation or excessive scar or granulation tissue.
Surgical Approach:
Surgery is performed as an outpatient under general anesthetic. Because the procedure involves surgically releasing scar tissue that may or may not encroach upon the bladder, urethra or rectum, your surgeon may recommend a pre-operative bowel prep. Under direct visualization, scars are released, allowing the well healed portions of the canal to be reopened. Dilators are used during the operation to check for improvement of the vaginal canal. Often, packing is placed after surgery to be removed in-clinic the following week.
Limitations:
Depending upon the degree of stenosis or cause, your surgeon may discuss likelihood of success. While we have had many successes, this surgery is difficult—far more difficult than maintaining a regular dilation schedule. Success long term will be estimated by your surgeon but is normally no greater than 50%. Your surgeon may predict a higher percentage if the obstruction is less. That said, patients often choose this method because it is relatively inexpensive and far easier to recover from than inpatient VDP, colon or robotic peritoneum surgery. This procedure relies on partial healing of the vaginal canal from the original GAV in order to be successful—something not always apparent before surgery. Those with excessive scar tissue may have limited benefit from surgery. Success can also depend on adherence to a dilation schedule after surgery.
Vaginal Deepening Procedures (VDP)
Regardless of the cause, vaginal stenosis can be a real problem. Before considering VRP,VDP, or RPFV, ask yourself why the loss of depth occurred initially and, if regained, what will you do differently? Do you need the vagina re-opened for sexual purposes or for your own sense of identity? Are you sexually active now or are you just hoping to expand your hypothetical options? Can you be faithful to a rigorous dilation schedule if depth is regained? Could you be ok with minimal depth if it means no further dilation routines and am still able to function sexually with my partner?
Under the assumption that conditions have changed and that patients are highly motivated to resume a dilation schedule that may have been abandoned, VDP involves re-dissection of the vaginal cavity and re-lining of the neovaginal cavity. Rarely, VDP can also be done for someone who never had depth after their initial vaginoplasty procedure and needs more depth for functional reasons.
VDP is a hospital-based inpatient procedure that requires a complete bowel prep in most cases and runs theoretical risks of visceral injury higher than with the primary GAV procedure due to internal scarring. These risks seem to be less when a robotic peritoneal approach is chosen.
Re-lining options may include skin grafting using excess full-thickness vulvar skin, abdominal or groin skin, or split-thickness skin grafts. Allograft materials (human donor–derived grafts), such as AlloDerm or DermaPure, are acellular dermal matrix products. Another increasingly utilized option is xenografting (non-human biologic material), most commonly derived from porcine or fish sources.
In most cases, grafts are incorporated successfully. True immune rejection is not a concern; however, in some patients a graft may fail to ‘take,’ which can result in partial or complete failure of the reconstruction. The robotic peritoneal flap approach reduces this risk, as it does not rely on graft material.
Ideal Candidate:
Suitable candidates at least 9-12 months out from primary surgery with stable limited depth who is motivated to follow rigorous dilation protocol.
Surgical Approach:
Some individuals have a previous surgical plane that can be re-dissected to return depth to the vaginal canal. There does appear to be less dissection risk when performed robotically rather than performed from below. benefit from dissection of the canal with robotic techniques and advancement of the peritoneal tissue in the abdomen to add additional depth to the vaginal canal.
Limitations:
Vaginal deepening procedure is NOT for someone interested in super human vaginal depth. Addition of the peritoneal approach requires utilization of a second surgeon, which can delay the procedure. Those with previous peritoneal flap or peritoneal pull through techniques would not be candidates for this procedure. After surgery, patients will have to follow a rigorous dilation schedule while the new vaginal canal heals.
III. Preparing for Surgery
Revision genital surgery is a surgery that will limit physical activity for typically 2-6 weeks depending on the surgery completed. A large part of its success depends on your preparedness. This means being in the best possible physical and mental health before the surgery.
Above all else, it is critical to have reasonable expectations about what is possible for your body and what your surgeon can realistically accomplish. We recommend you:
- Speak with a mental health professional who has an understanding of gender care to help navigate these nuanced choices in addition to consultation with your surgeon
- Connect with peers who have been through this surgery for support. Please keep in mind that each person’s surgical plan and experience is unique. Information shared on some online forums may not be relevant to your surgery. Due to patient privacy laws, we never comment on another patient’s specific issues or experiences. We are happy to clarify anything related to your individual care.
Maximizing Healing
We like to think abouts urgery like running a marathon. You will be stressing your body and will haveto do significant healing. In the weeks to months before surgery, maximizing your health–both mental and physical–will help you recover more quickly. To maximize healing, we recommend:
- Getting roughly 0.5 gram of protein per weight in lbs a day to maximize healing (e.g. 150lb x 0.5=75g of protein per day).
- Reducing sugar and processed foods.
- Remaining active before having surgery. Keeping up with or adding a workout plan will benefit your overall health and support a speedy recovery. Examples can include adding daily walking, home yoga, or simple home workouts with body weight to your weekly routines.
IV. Planning for Recovery
We understand the importance and urgency of this surgery. We also know your success hinges on being well-prepared. Remember, this is a lifelong investment in your health. Optimal preparation can improve your chances of positive physical and mental health outcomes.
- Home support: In addition to assistance with food, transportation, housework, and running errands, you will require assistance from your caregiver with activities that involve lifting more than 10 lbs. Additionally, you might need support with caring for pets or children.
- Emotional support: You will need emotional support, while healing and while you have limited mobility. Think about what coping strategies you can use during this time.
- Housing
- Utilities
- Groceries
- Medical supplies and medications
- Other bills and expenses
- Make a backup plan in case you need more time to heal.
- Find out if you are eligible for Family Medical Leave through your employer. Get your paperwork in early.
- Insurance status
- Moving or loss of housing
- Loss of income and financial concerns
- Different caregiver(s)
- New health condition

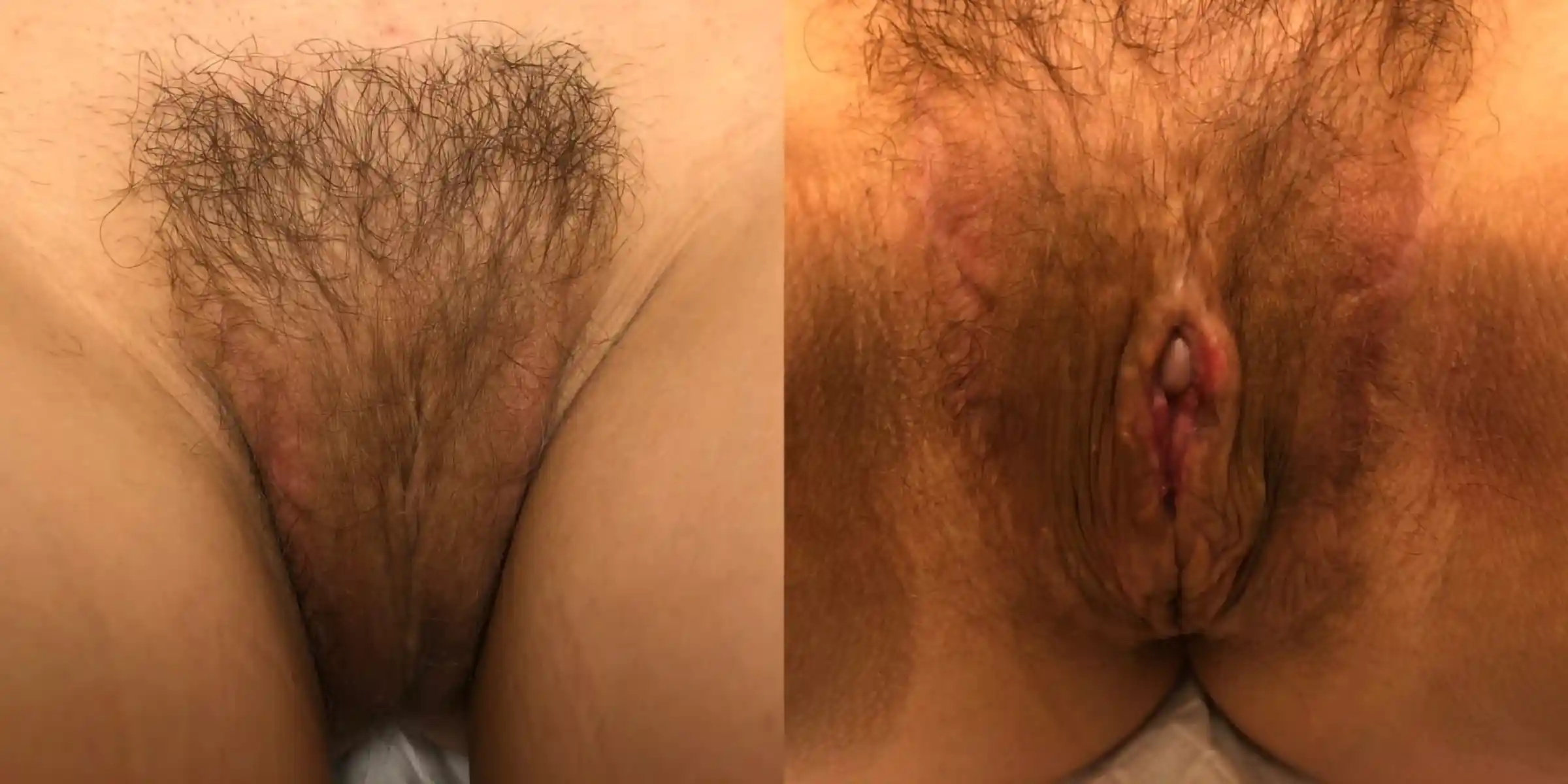
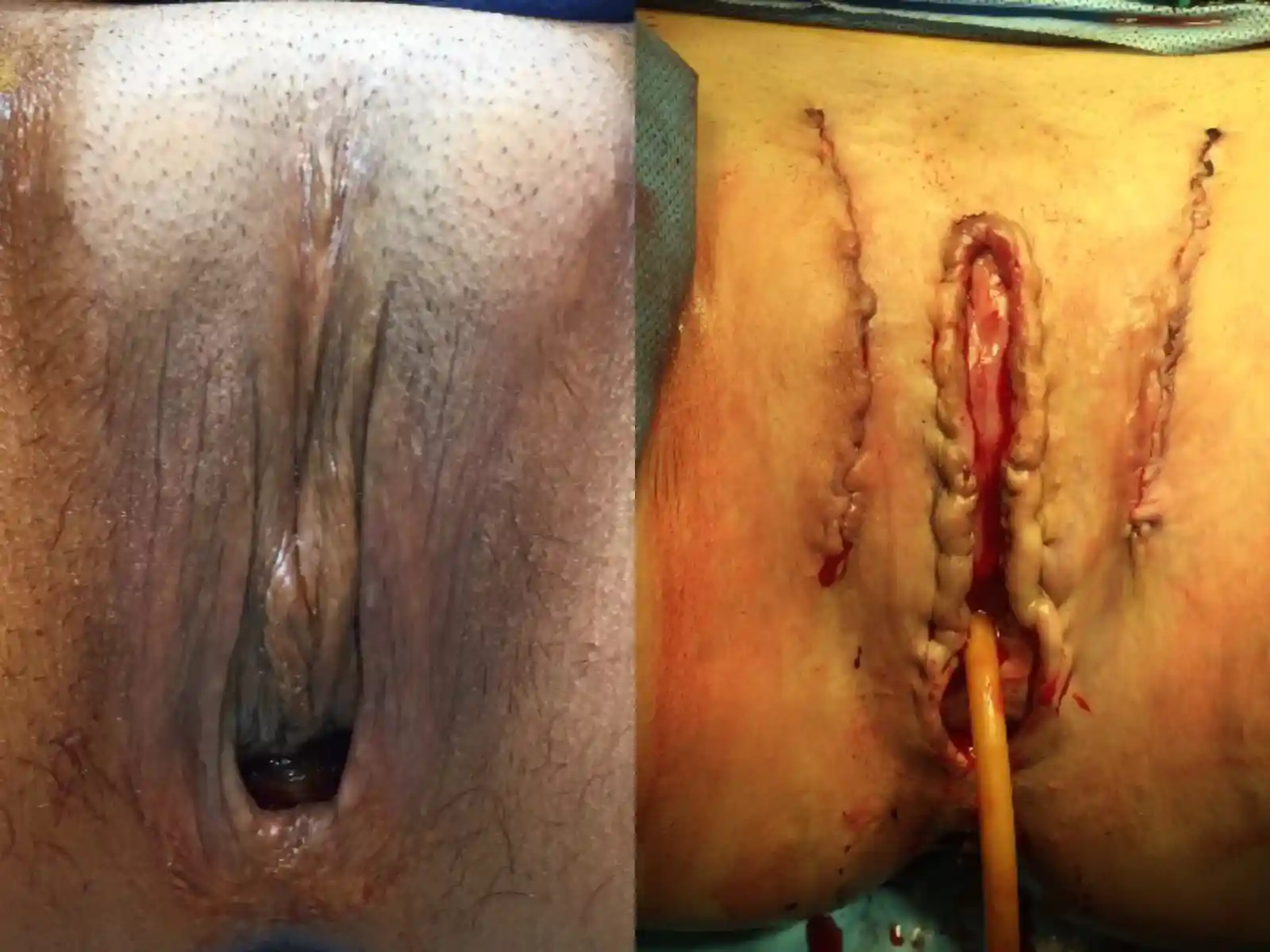
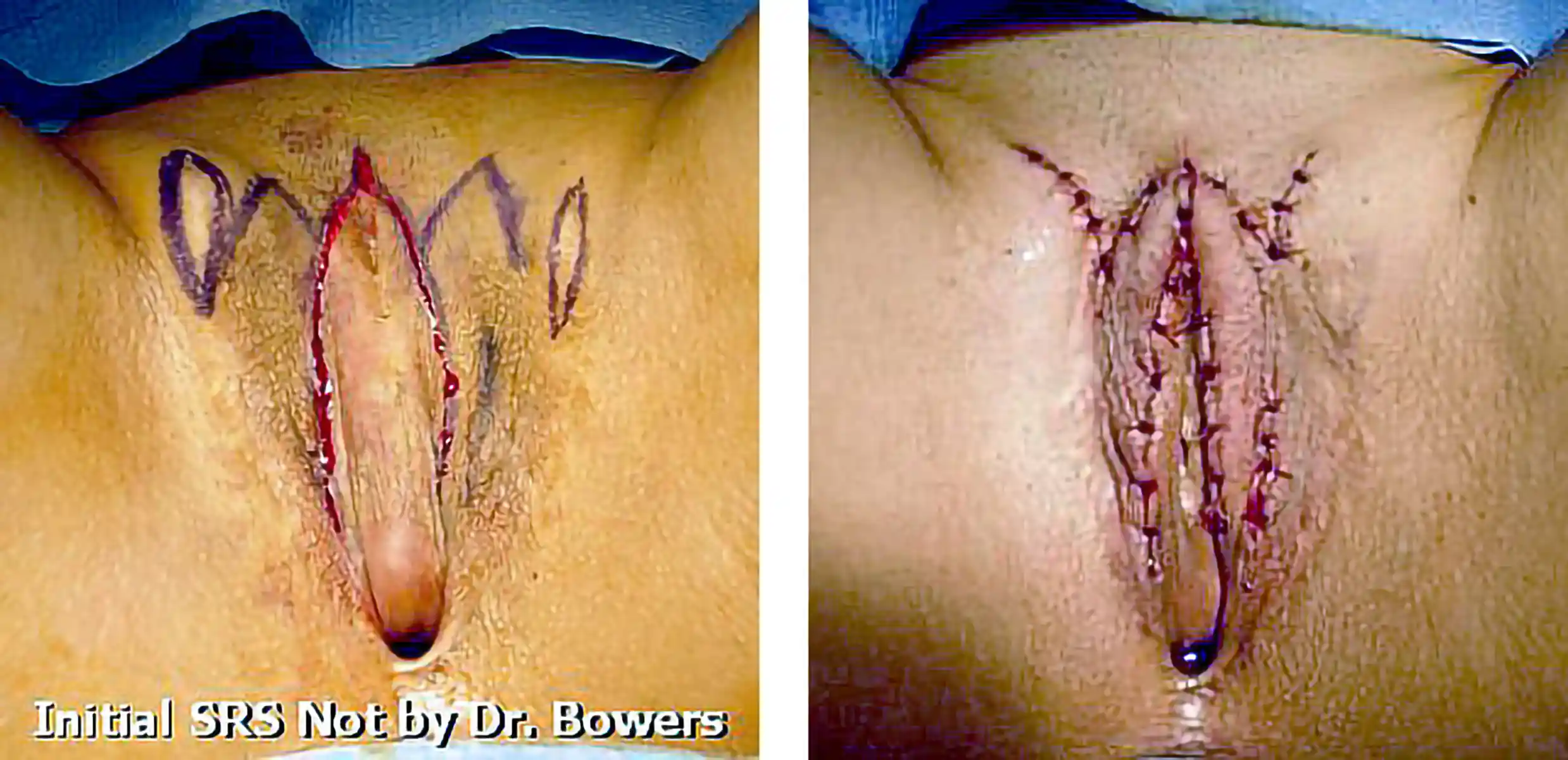
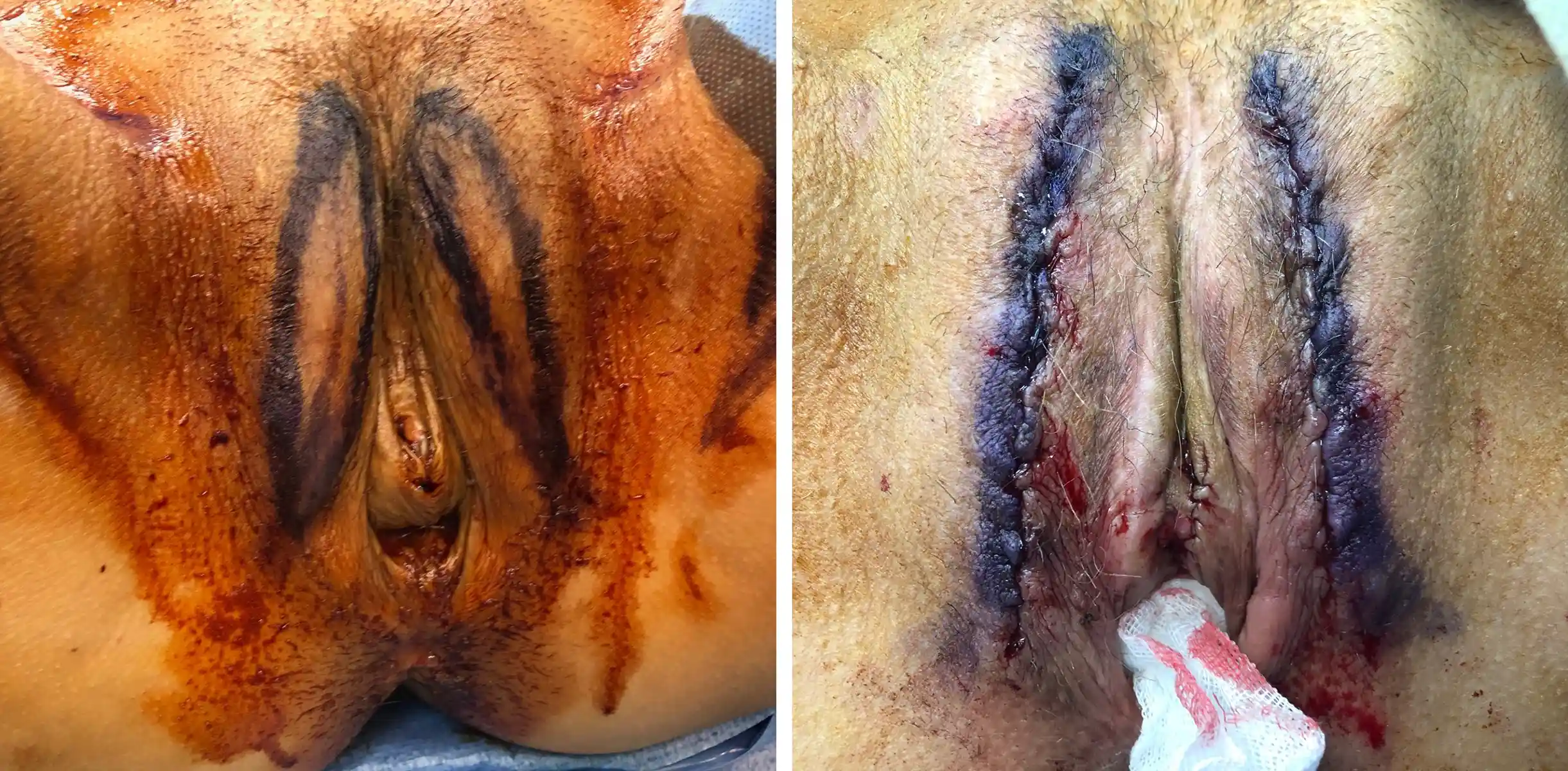
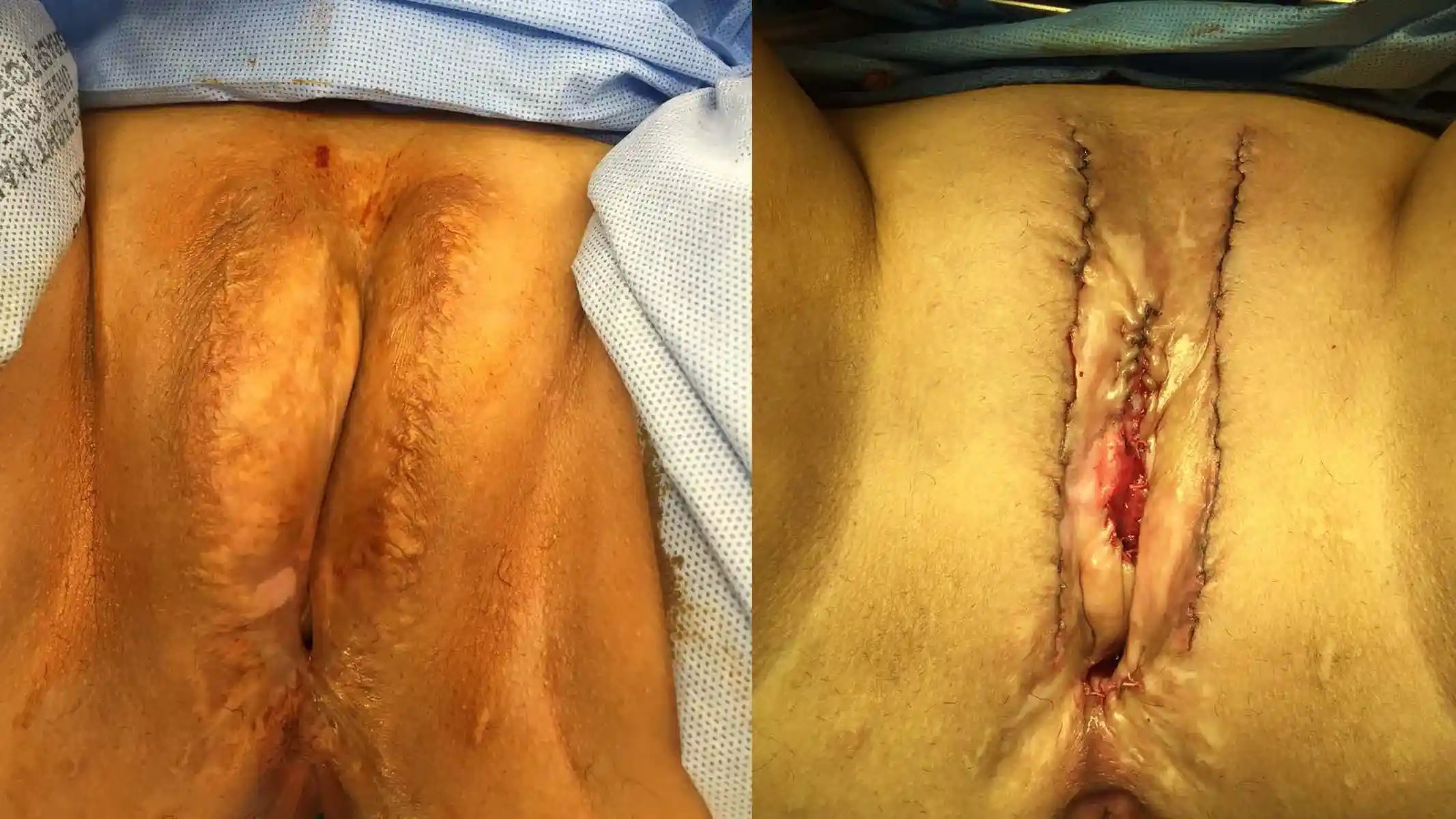
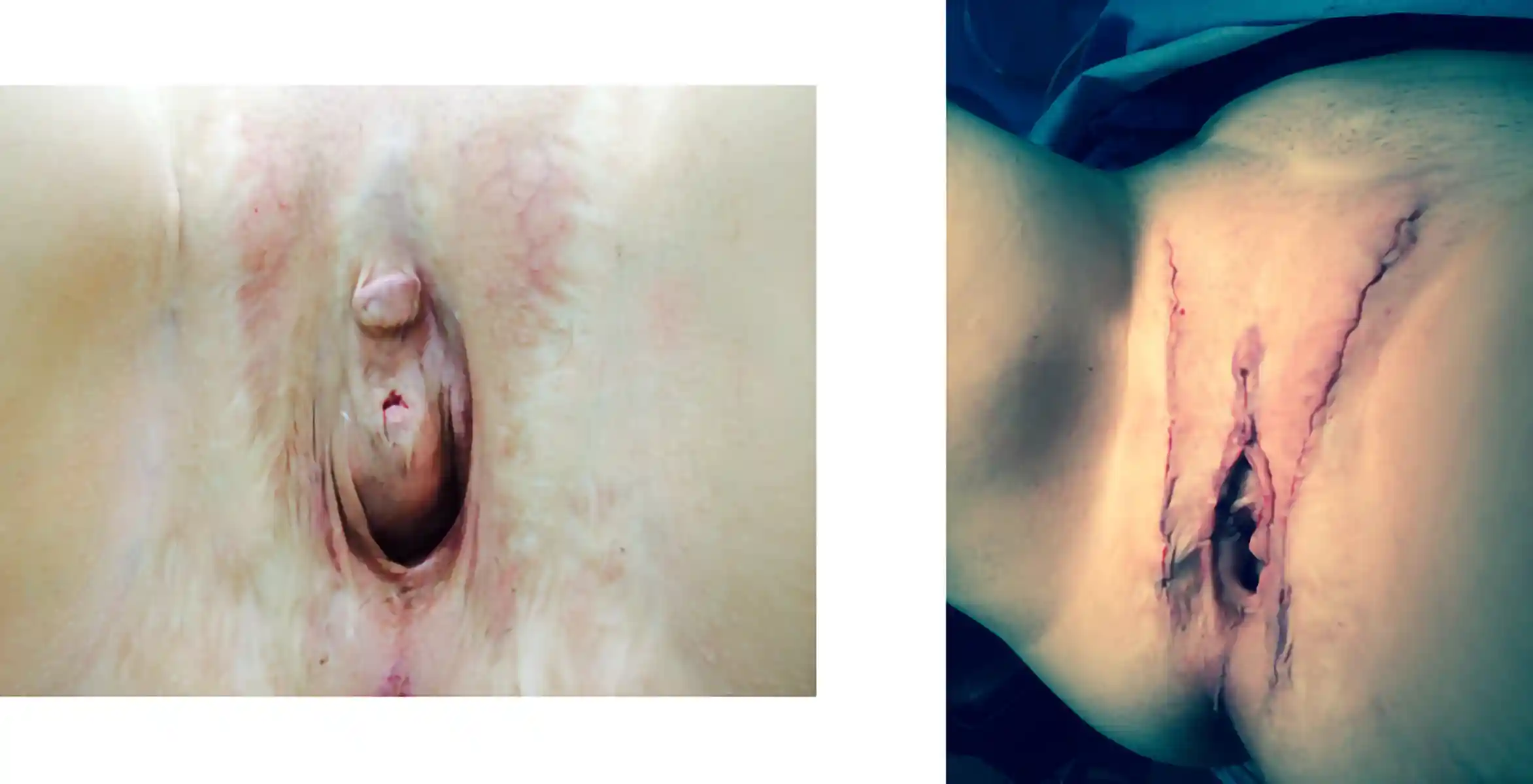
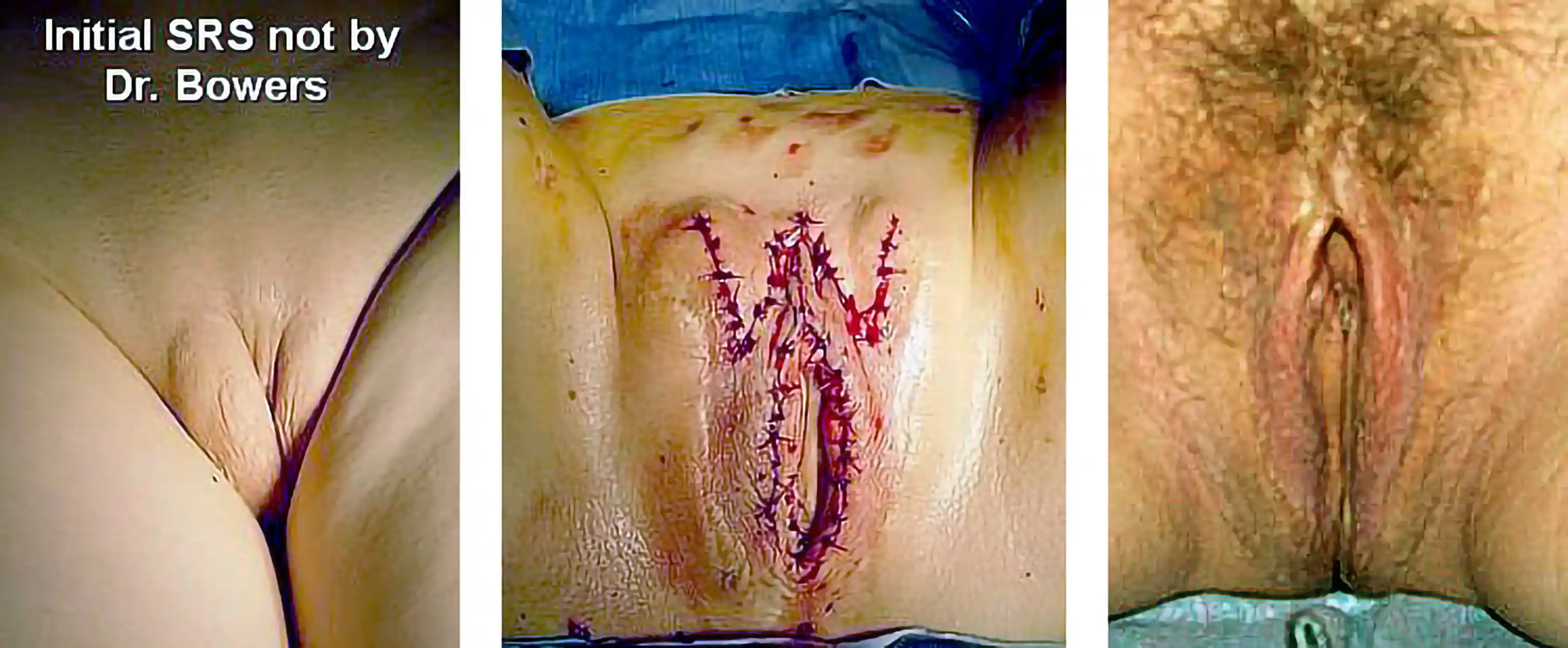
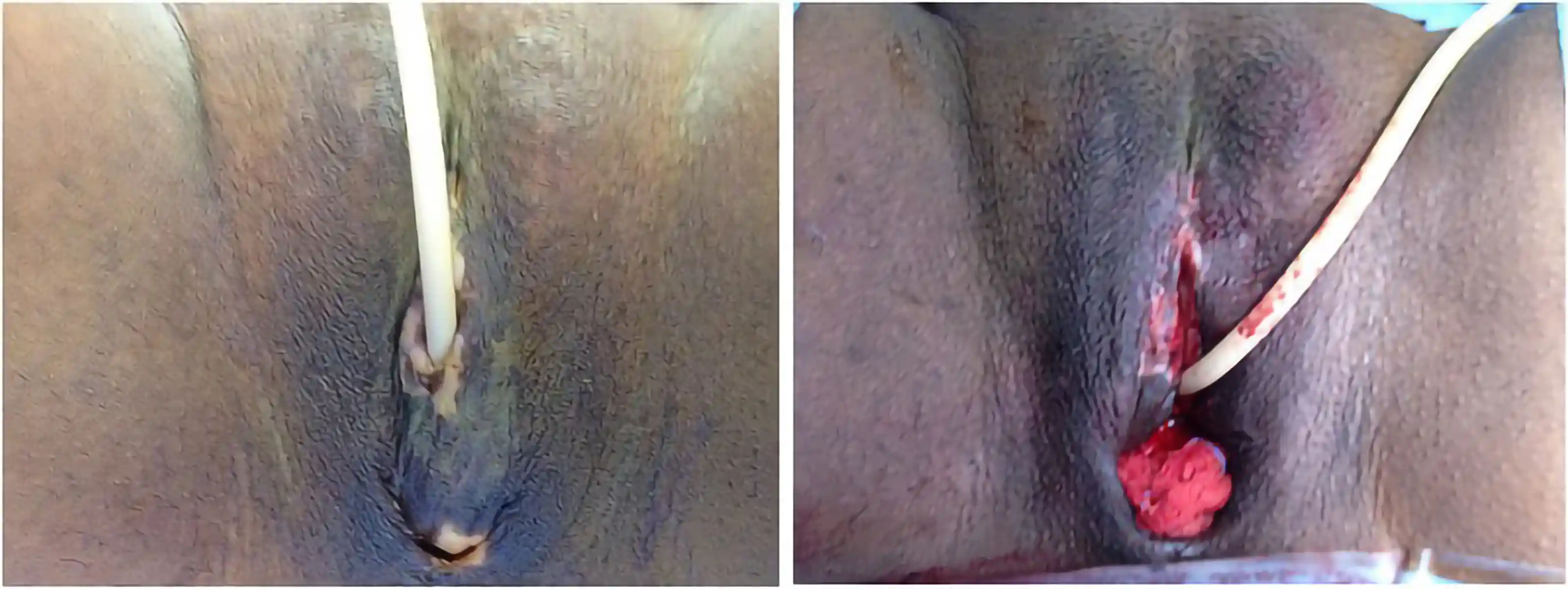
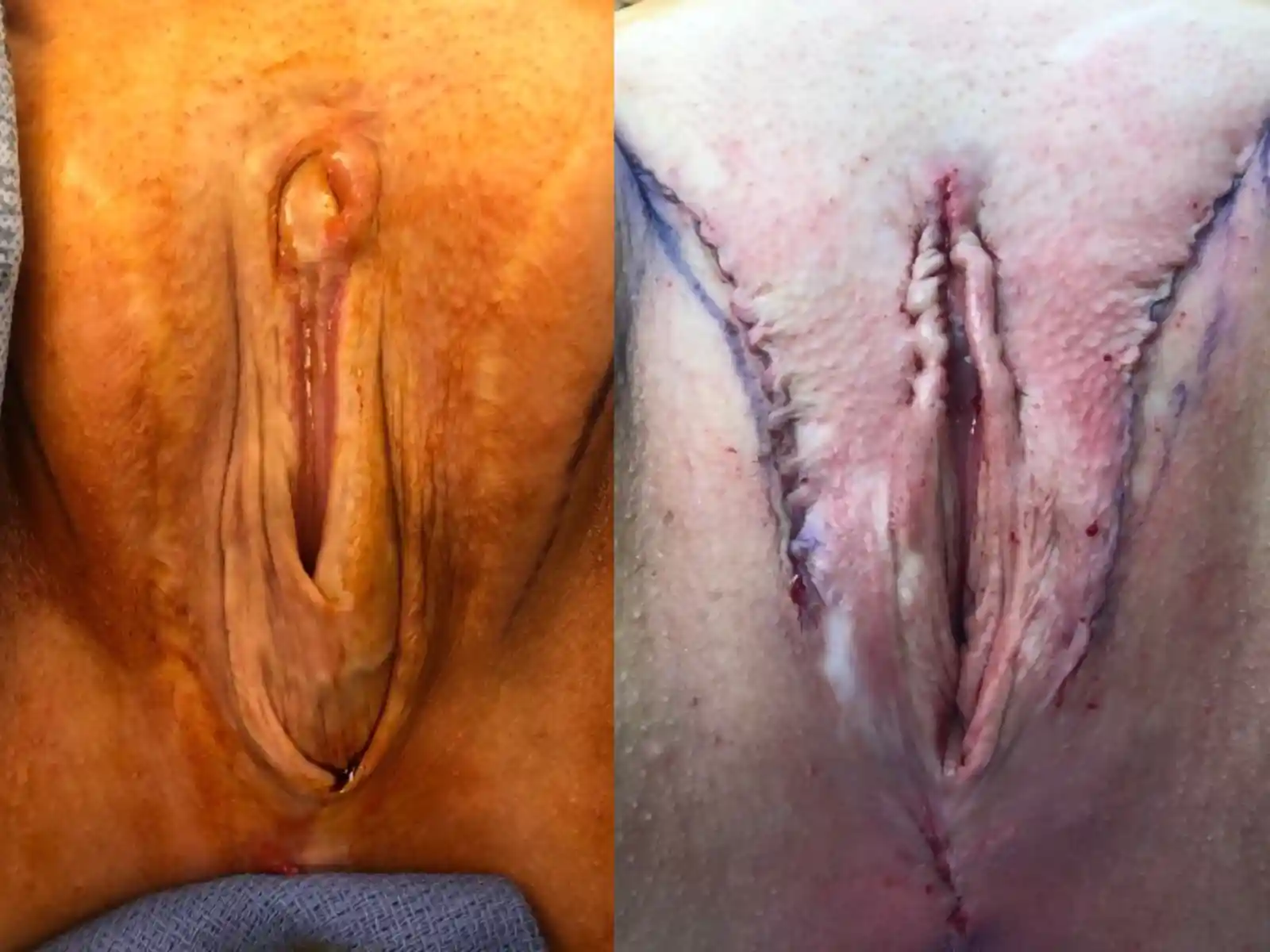
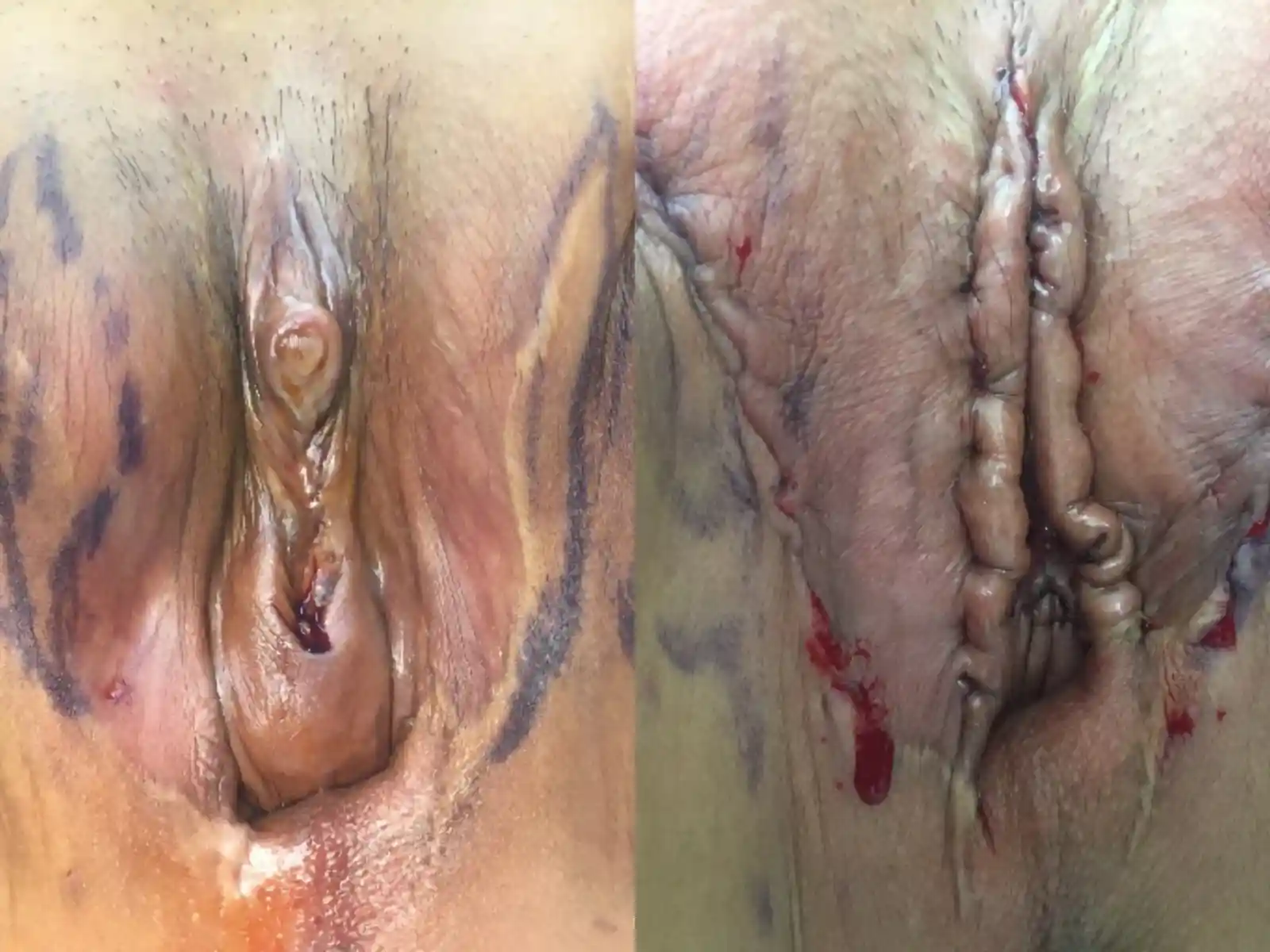
![[Left/Center] Prior vaginoplasty plus three labiaplasties and grafting by another surgeon left severe vaginal entry scarring, exposed and anteriorly displaced clitoris, and asymmetry. [Right] Dr. Bowers performed bilateral scar revisions, fat transfers, hoodplasty, and clitoroplasty to restore symmetry and contour while maintaining patient-requested depth.](https://cdn.prod.website-files.com/693cb6ff51584191bed8f2c2/693cb6ff51584191bed8f5eb_uc.webp)