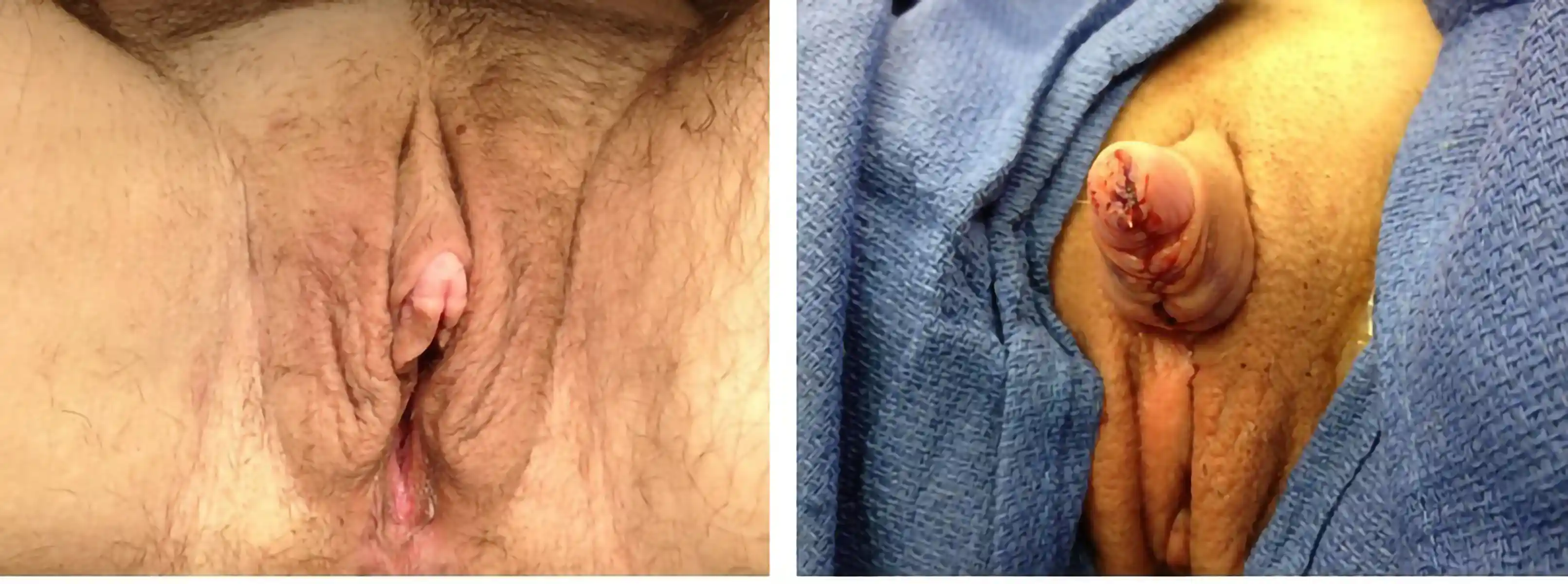
Genital Masculinizing
Welcome to Legacy Surgical Partners – we look forward to caring for you! Our priority is to make your surgery process and everything in between as pleasurable, empowering, and accessible as possible. Patients are expected to follow guidelines established by the WPATH Standards of care Version 8. We follow these standards—not as a gatekeeping hurdle—but as minimal guidelines that are useful guideposts that are protective. Though regret for gender affirming surgery is extremely rare, we are medical professionals who are here at your bequest. Surgery is irreversible, which puts the onus of responsibility on both patient and provider.
We're here to help you make essential decisions and know what to expect in surgery planning and recovery. Our team consists of:
- Surgeons
- A physician assistant
- Medical assistants
- Our surgery scheduler
- Office team
- And you
That’s right, you! We value your input, your perspective and all the work you are and will be doing to prepare for and recover from surgery. We look forward to getting to know you better and learning how we can help you.
We want to make your surgery and recovery as smooth as possible. We’ll answer questions you have and make sure you have the best possible outcome.
I. Metoidioplasty Overview
We know this surgery is extremely important. It takes incredible trust to allow a surgeon to perform this operation. We want you to know we are humbled by that trust and take it very seriously.
The first step in this complex process is understanding your options and creating a plan that meets your needs. We’ve created this overview to help you make important decisions and know what to expect.
What is metoidioplasty surgery?
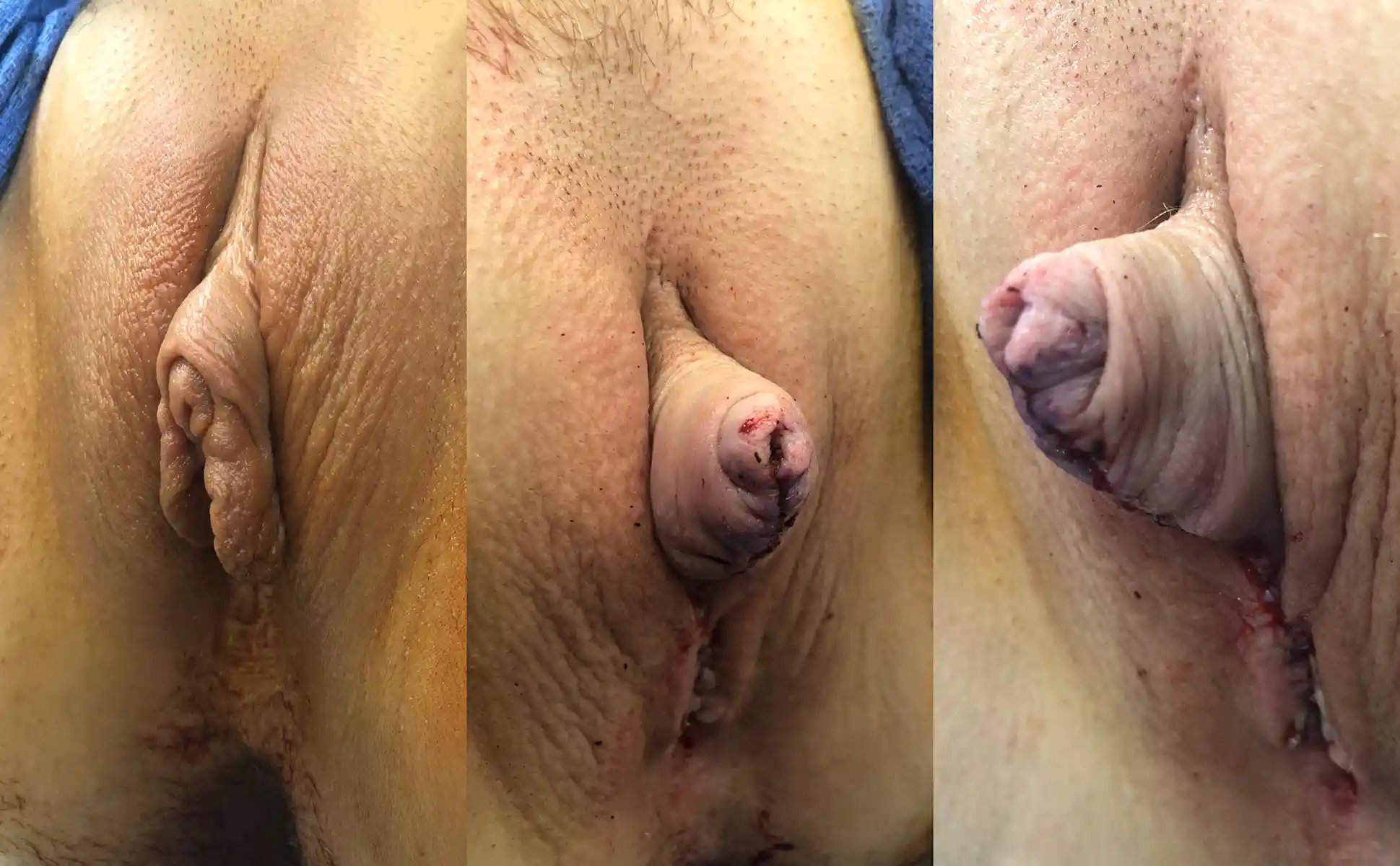
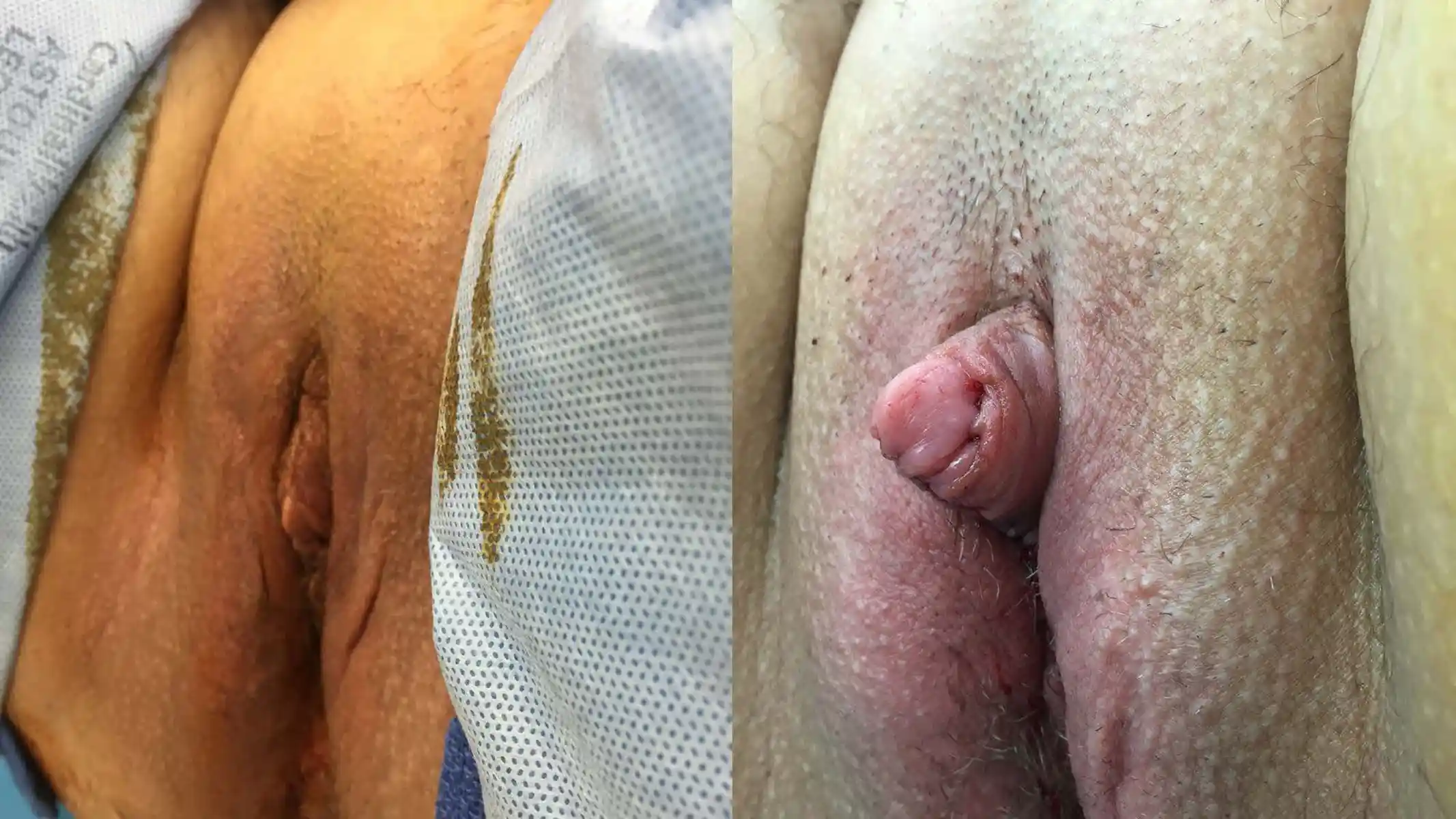
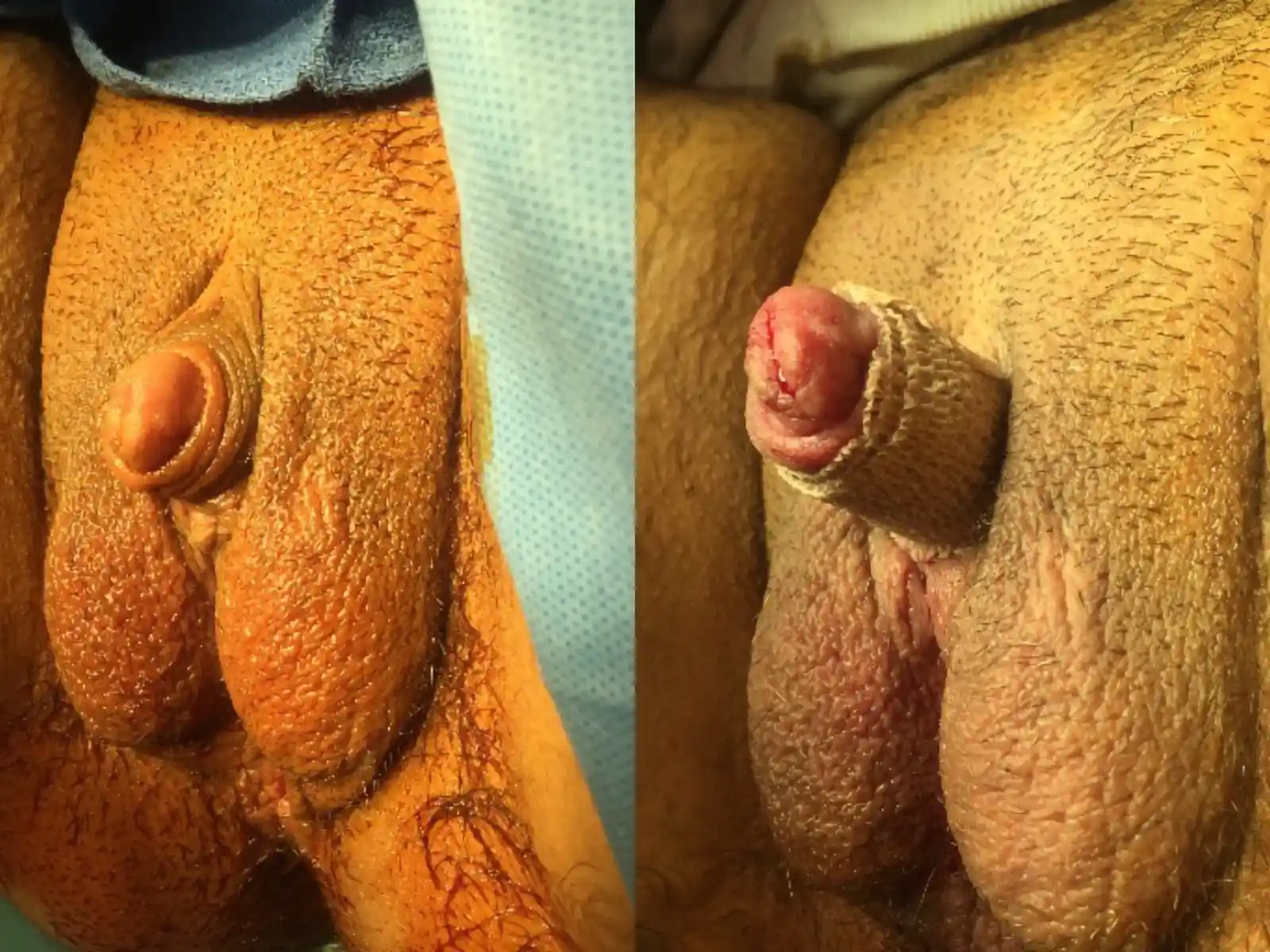
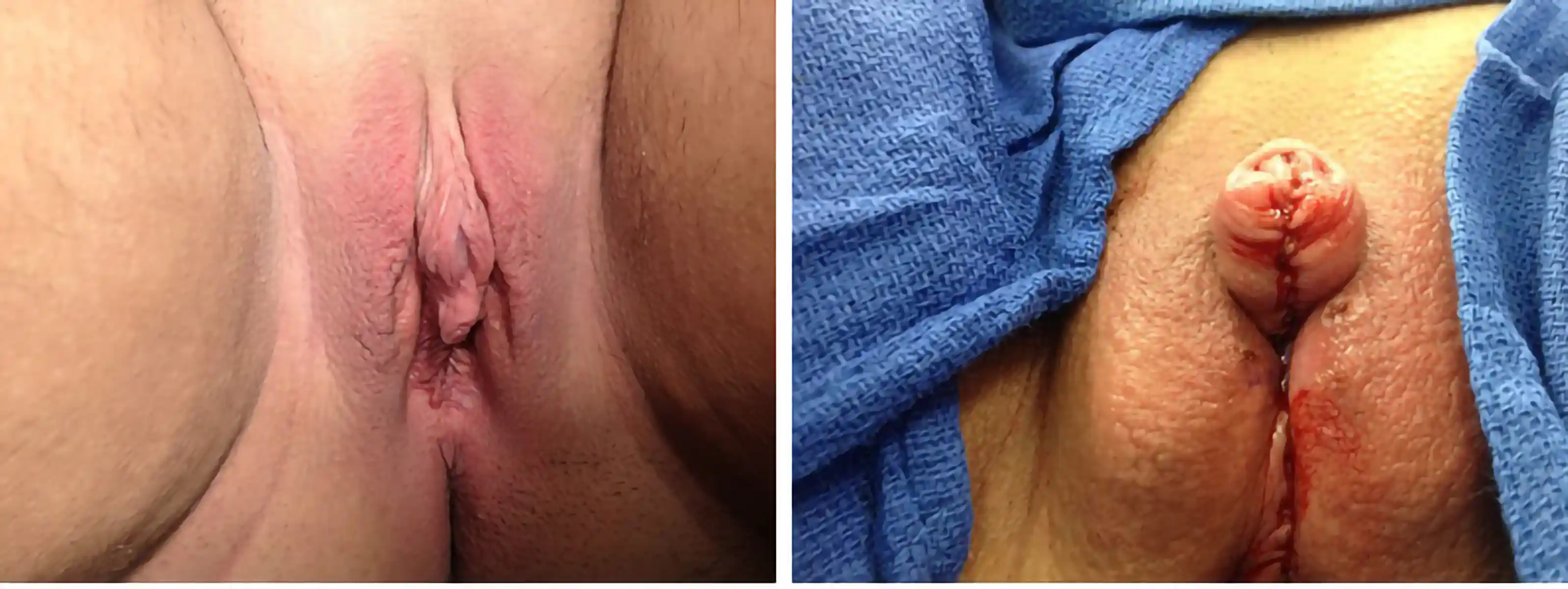
Metoidioplasty (in Latin, “becoming male”) is a procedure in which we aim to both lengthen your penis and position it to be more forward-facing while maintaining full sensation. This procedure can be combined with urethral lengthening, scrotoplasty, hysterectomy and/or vaginectomy. Testicular implants and scrotoplasty, should these be desired, are accomplished in a second outpatient procedure. Goals:
- Give penis more length by releasing ligament attachment .
- Position penis to a more forward position.
- Remove, reposition, reshape local tissue to make penis more visible.
Each patient’s surgery and results are different.
II. Before Surgery
Before your first consultation, we encourage you to:
- Consider your goals and priorities for surgery.
- Write down your questions and bring them with you to your visit.
- Consider a support person to come with you. Ideally, this would be the same person who will care for you after surgery.
Your First Consultation
Your first consultation is an opportunity for us to learn about your hopes and goals. You may be given a questionnaire to help us meet your needs and measure the results. Your surgeon will review various surgical options and explain the process.
Once we understand your goals, we will:
- Evaluate your anatomy.
- Take pre-operative pictures.
- Assess your overall health to see which surgeries can meet your goals.
A fair amount of time is spent during the consultation with your surgeon, but you may also meet the other members of your care team.
Metoidioplasty Options
Simple Metoidioplasty
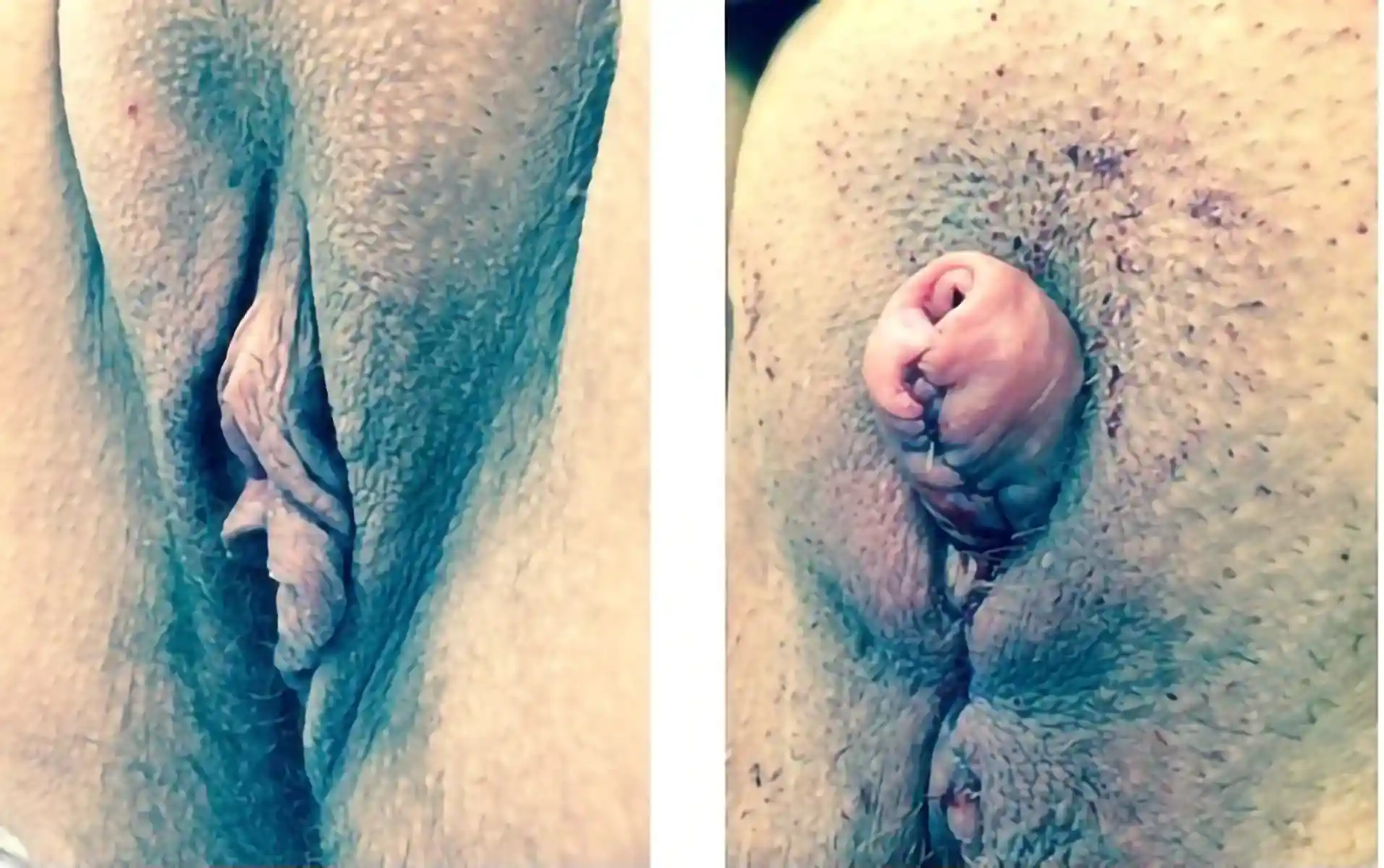
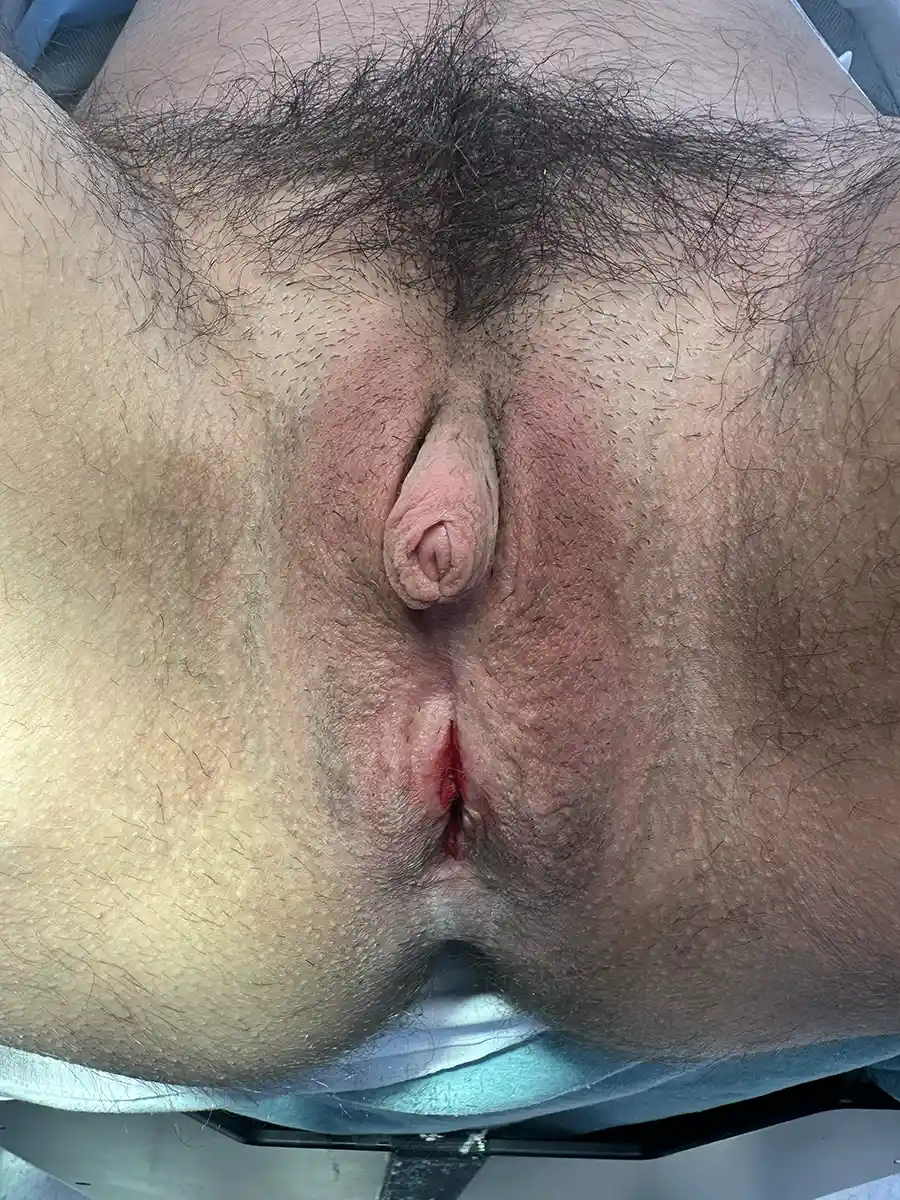
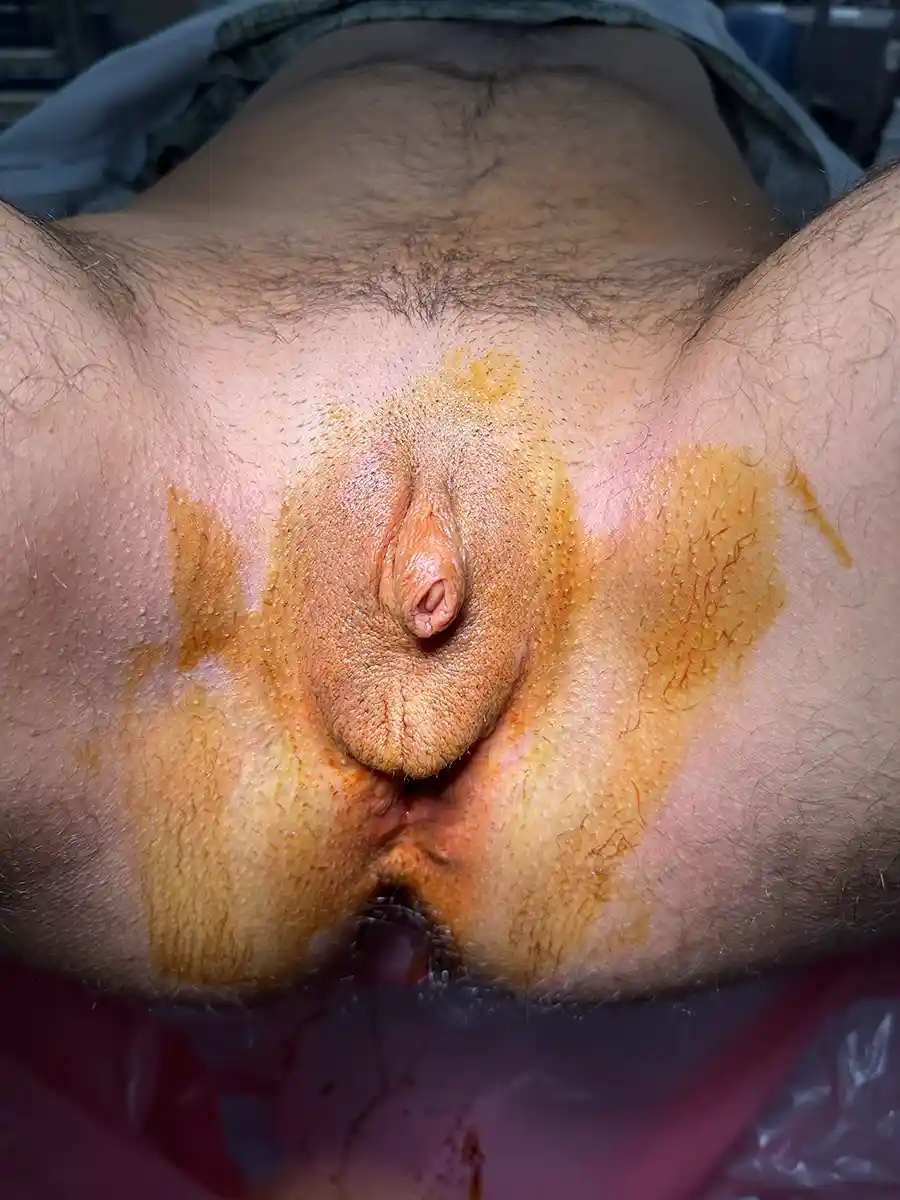
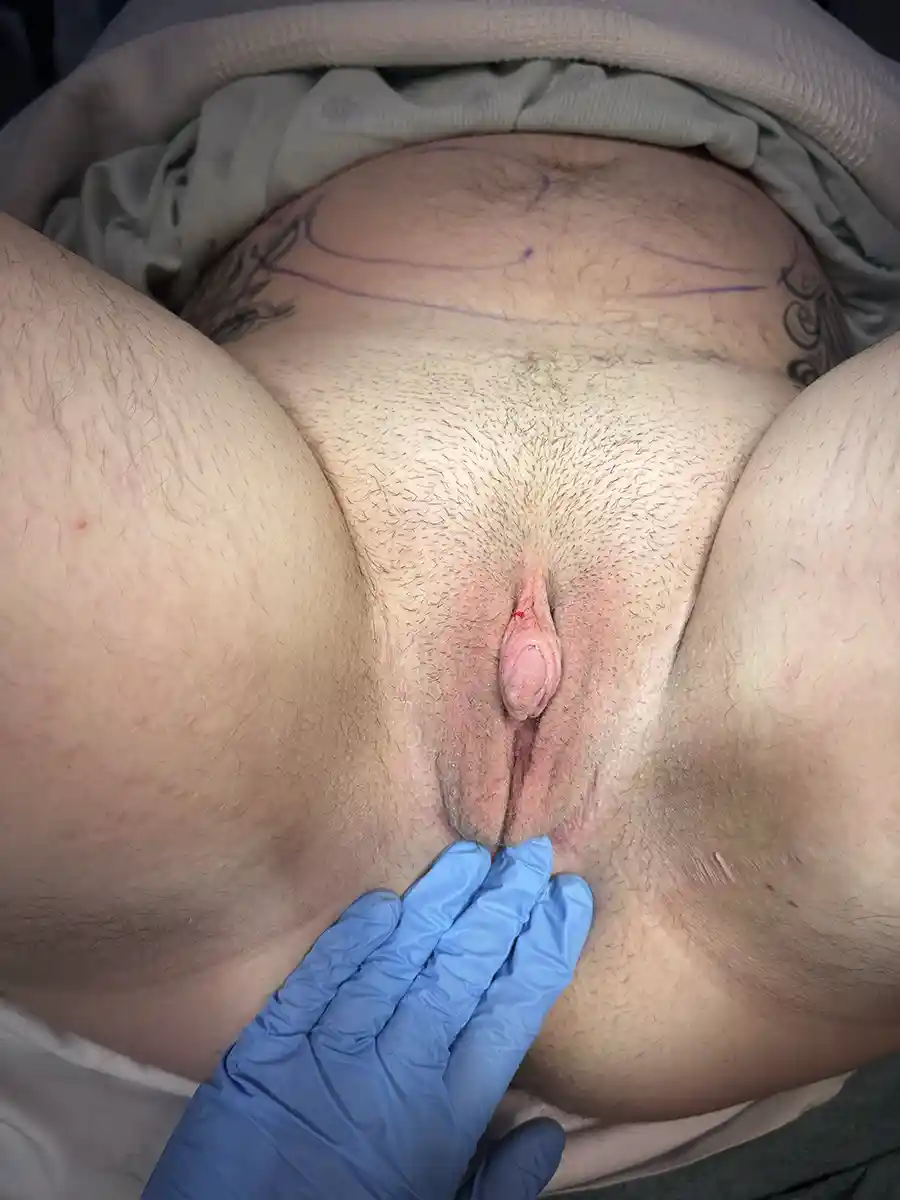
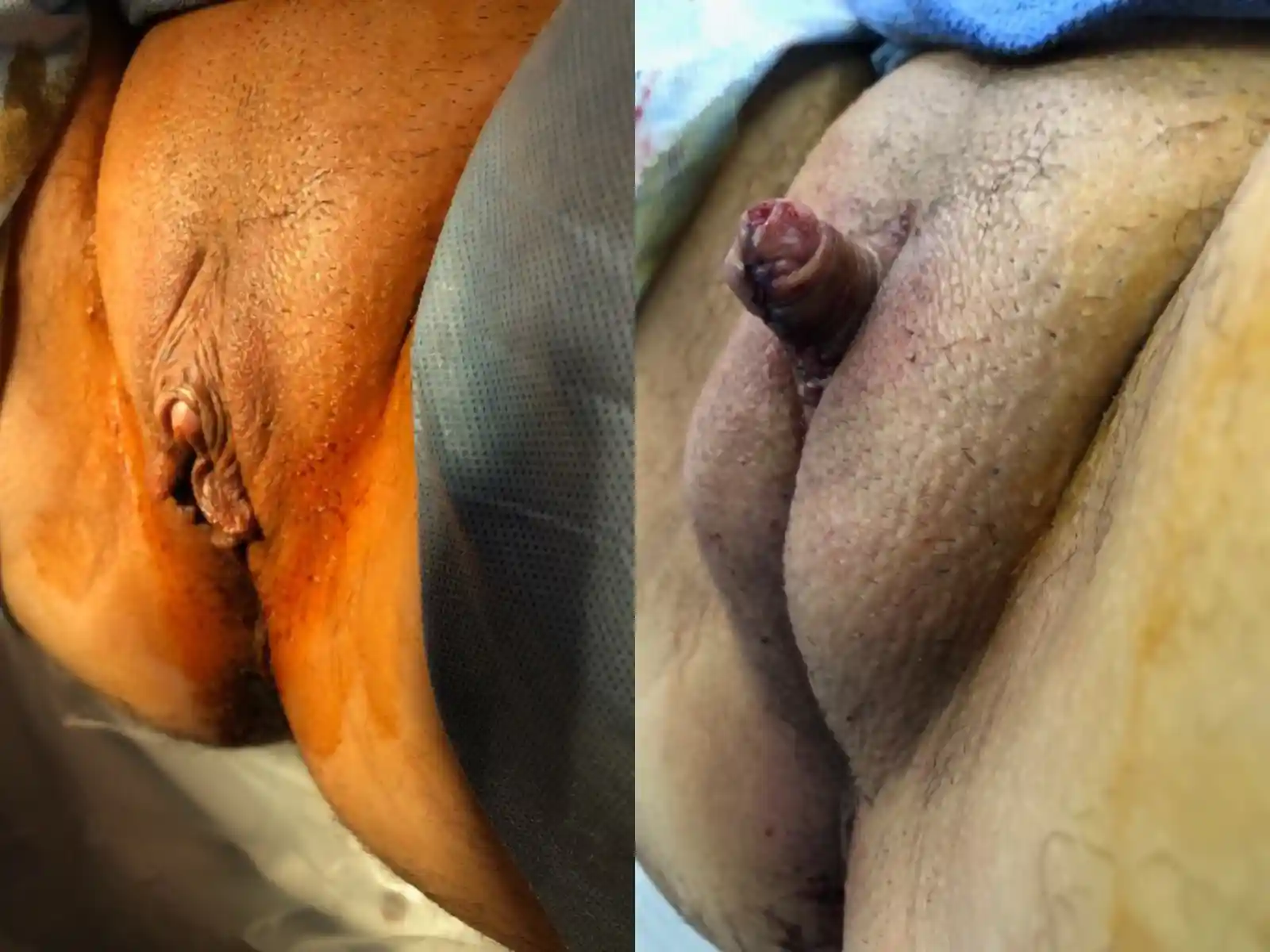
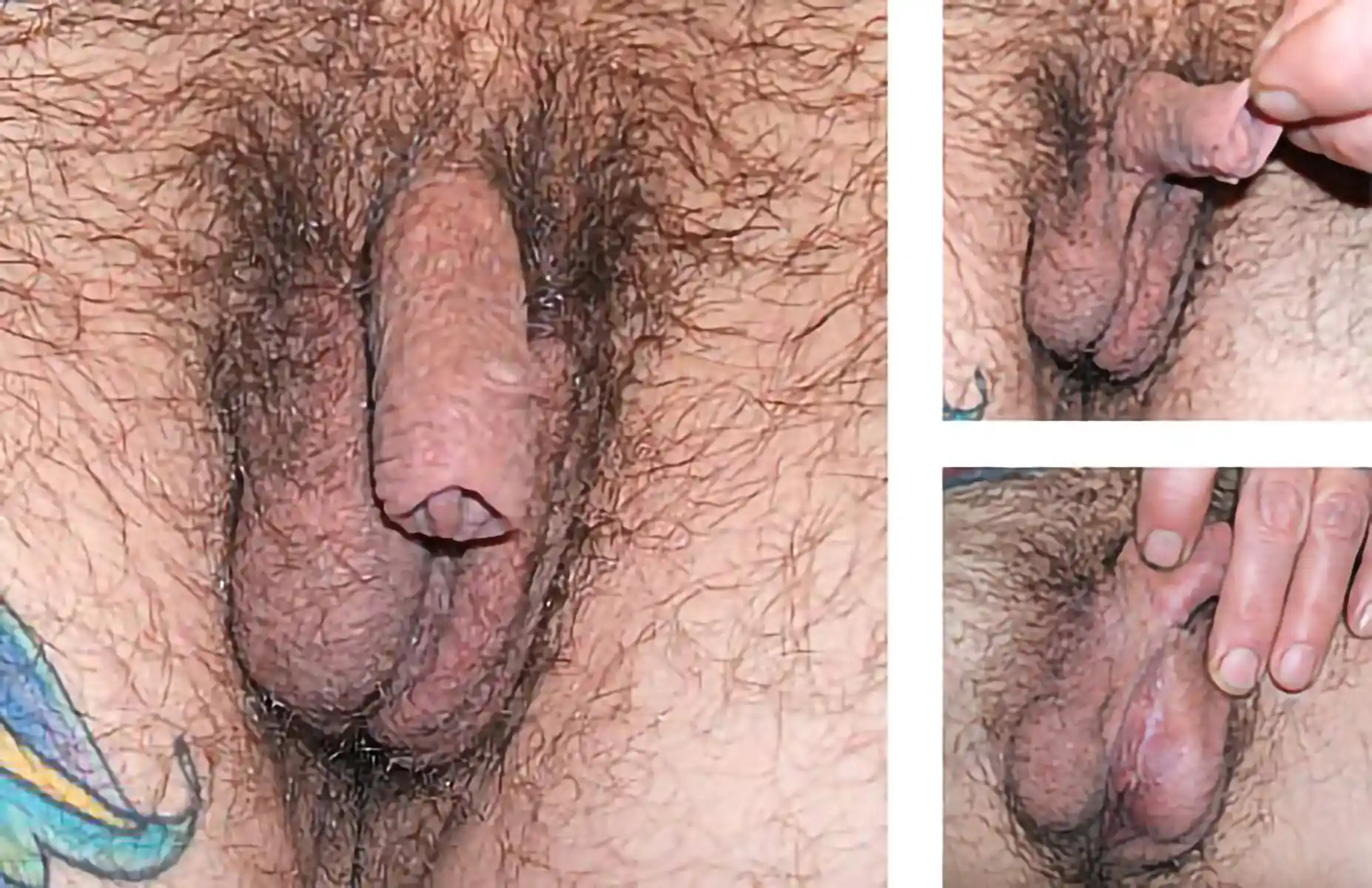
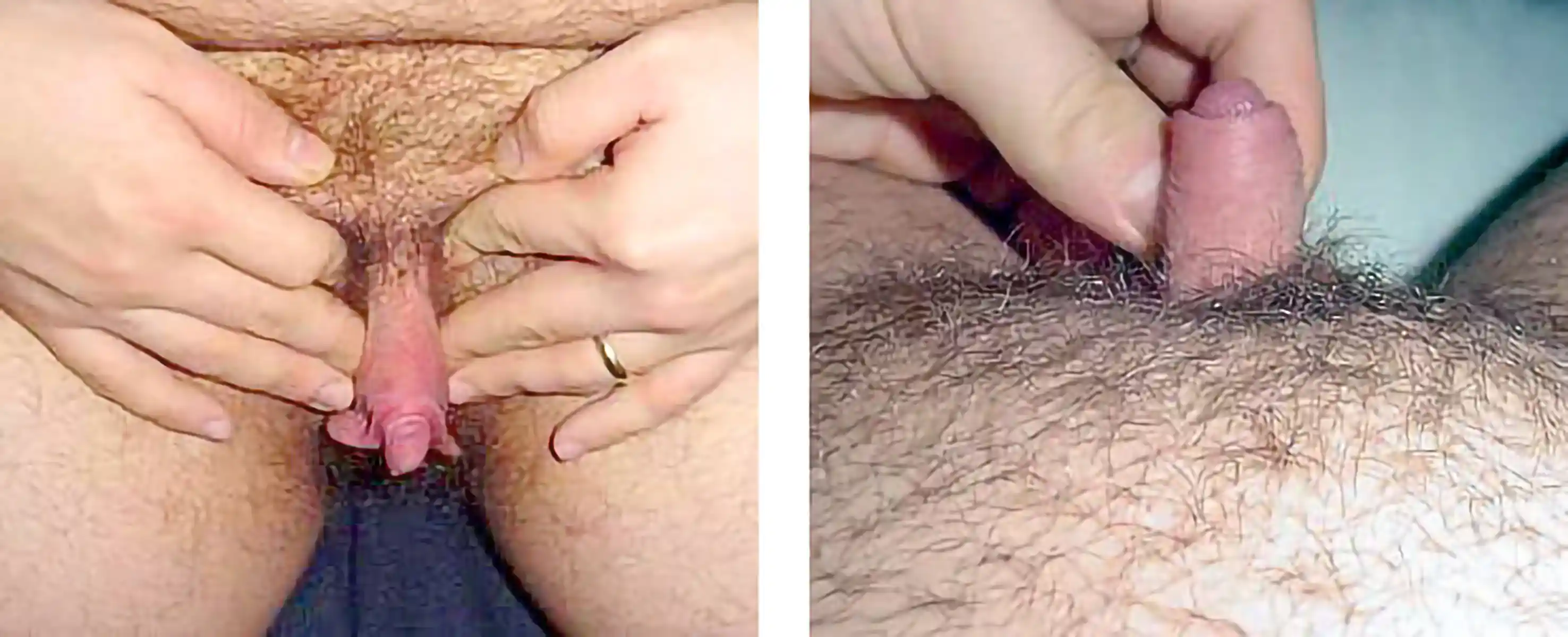
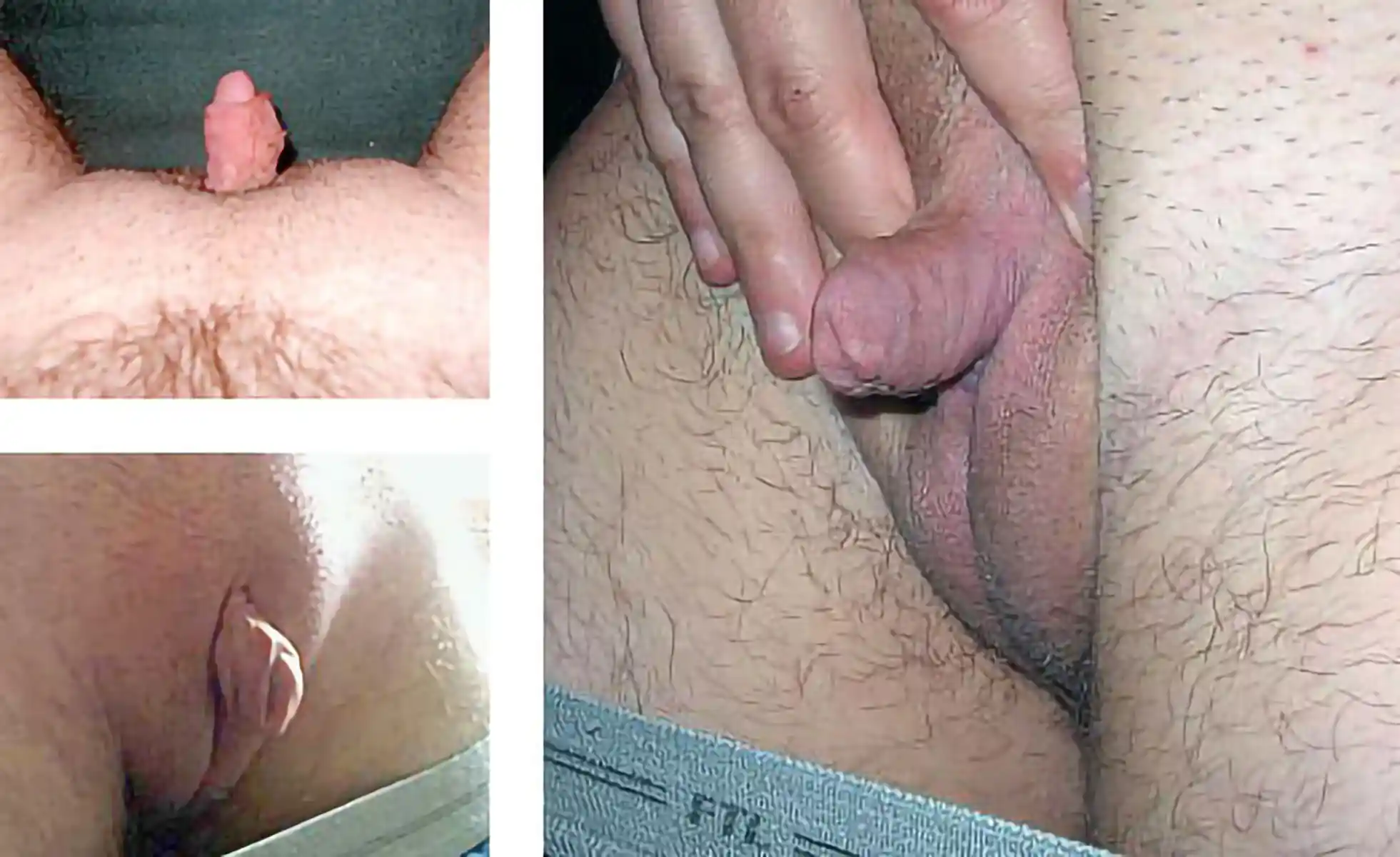
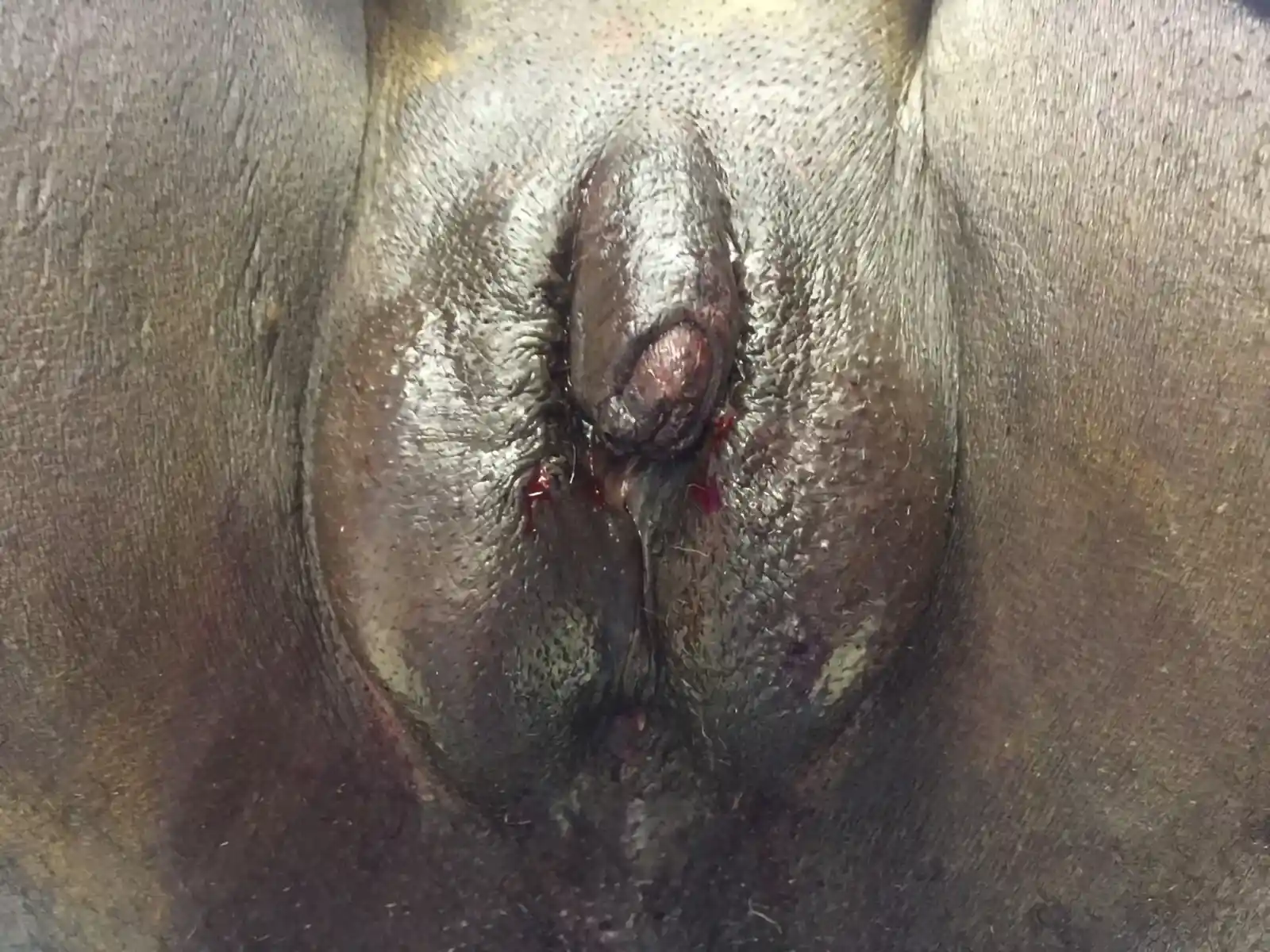
This is by far the most common technique for metoidioplasty. In this operation, the inferior ligaments are released, allowing the penis to come forward and rotate up. This gives more length and makes the penis more visible. The labia minora attachments are released, reconfigured or removed to give more framing to the penis. This can be combined with other procedures. Of note, Dr. Bowers was the first to describe the simple meta in 2004.
Ideal candidate:
Someone at a stable weight with enlarged penis from testosterone.
Limitations:
Those with lesser enlargement of the penis will have less of an improvement. Those with large amounts of groin, mons or lower abdomen fullness may not notice results. Your surgeon will discuss your specific anatomy with you. Monsplasty (reduction of the fat mound above the pubic bone) is an option at a future date that some patients choose if the mons obscures the penis—monsplasty can help.
Scrotoplasty w/wo Implants
Often combined with metoidioplasty, this procedure repositions the labia majora to create a scrotum. Depending on the chosen surgical approach, testicular implants can be placed at the same time or as a secondary procedure in the future.
The simplest approach is to place implants into the existing tissue with a minimal amount of tissue rearrangement. The advantages of this technique are that implants are placed and no second stage is needed. The disadvantages are that the scrotum is separated and implants can be a bit high-riding. Some will have a revision surgery to unify the scrotum as a second stage.
In a more common approach, the scrotum is created by making flaps (a surgical term for tissue that is moved to a new location) from the lower portion of the labia majora and bringing them centrally to make a cohesive scrotum. This constructs a scrotum that is well-formed beneath the penile shaft. We allow this to heal and then the implants are placed during a second surgery after about 3 months. The second surgery can be combined with a V-Y advancement in which the upper portion of the labia majora is lowered to provide further projection of the penis, adding volume to the scrotum.
Ideal Candidate:
Someone at a stable weight looking for creation of a scrotum.
Limitations:
The size and shape of the scrotum is dependent on your anatomy and will be different from person to person. Your surgeon will discuss your specific anatomy and goals.
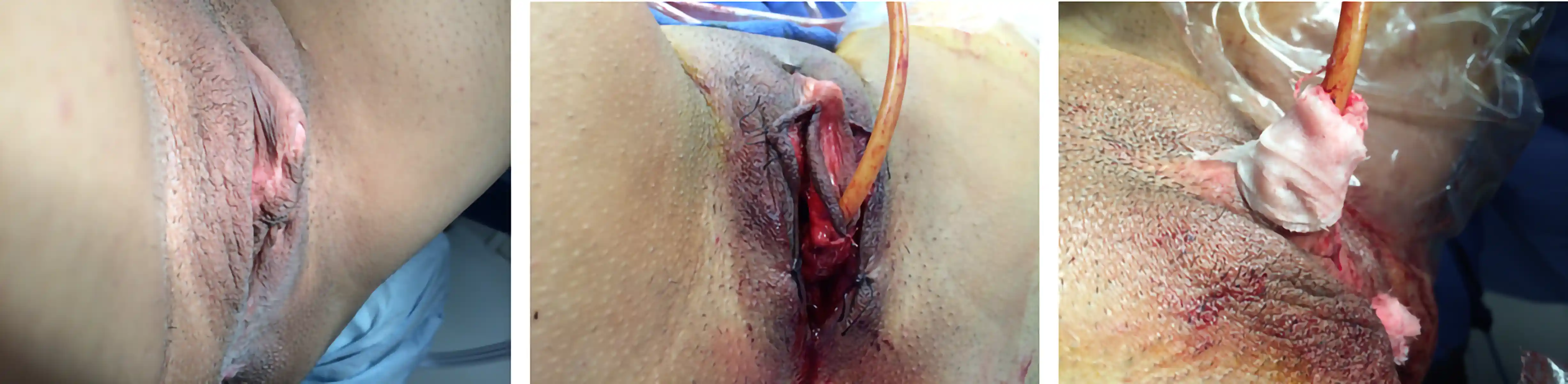
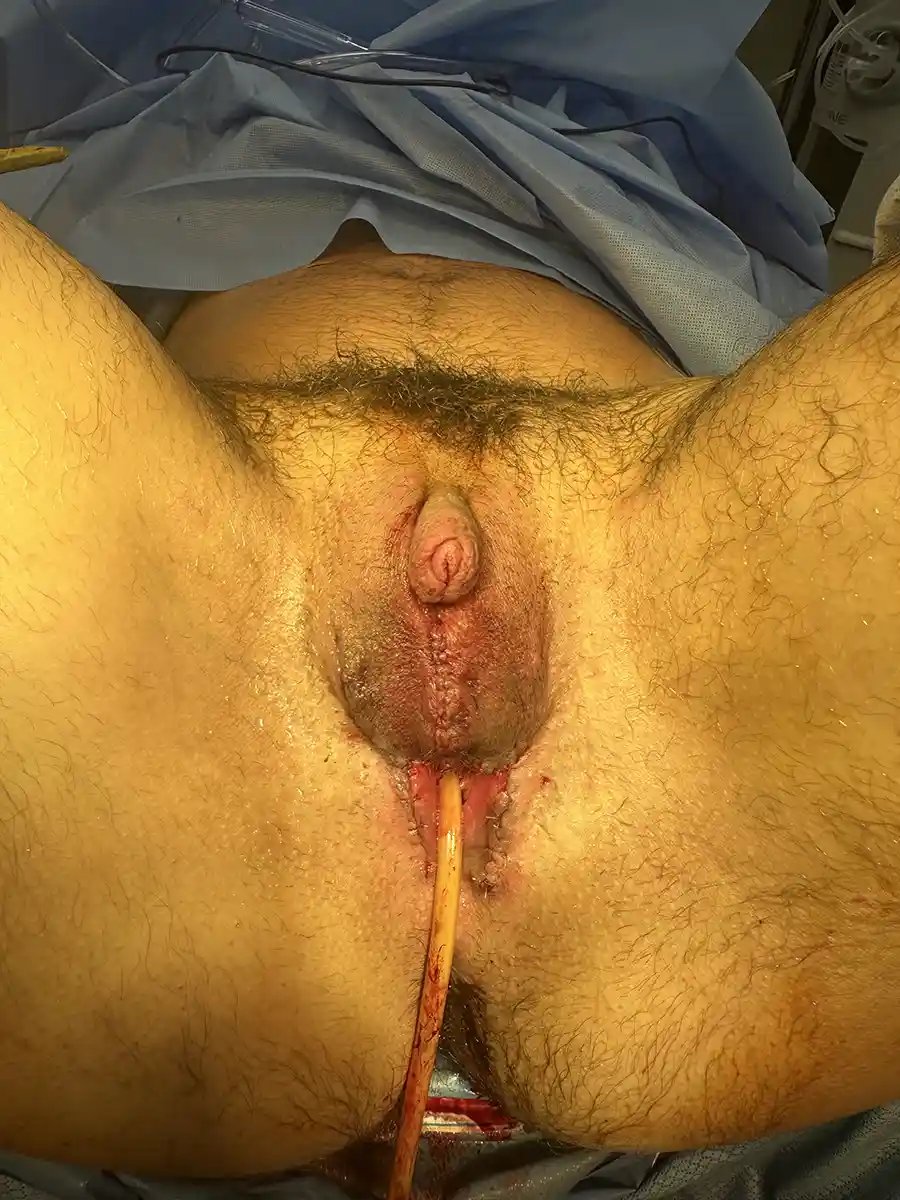
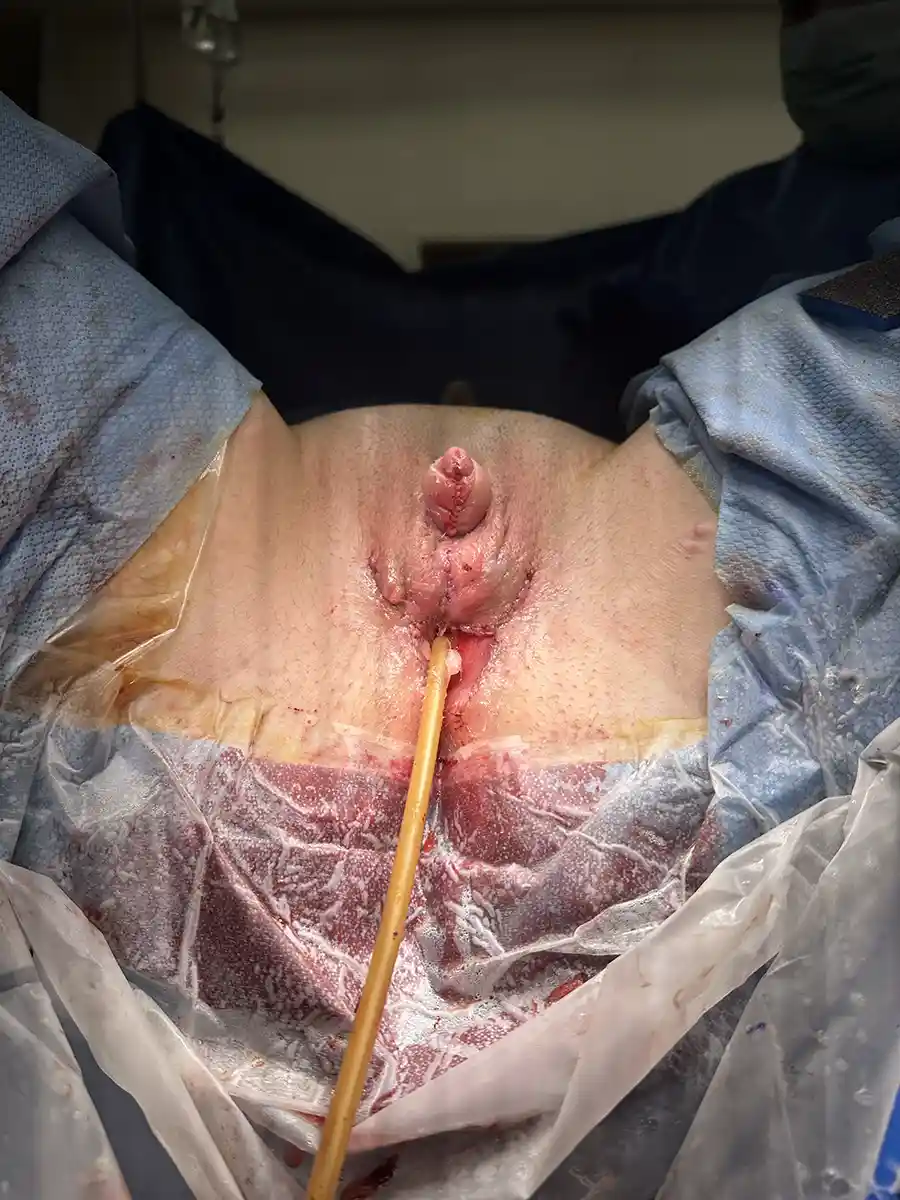
Urethral Lengthening
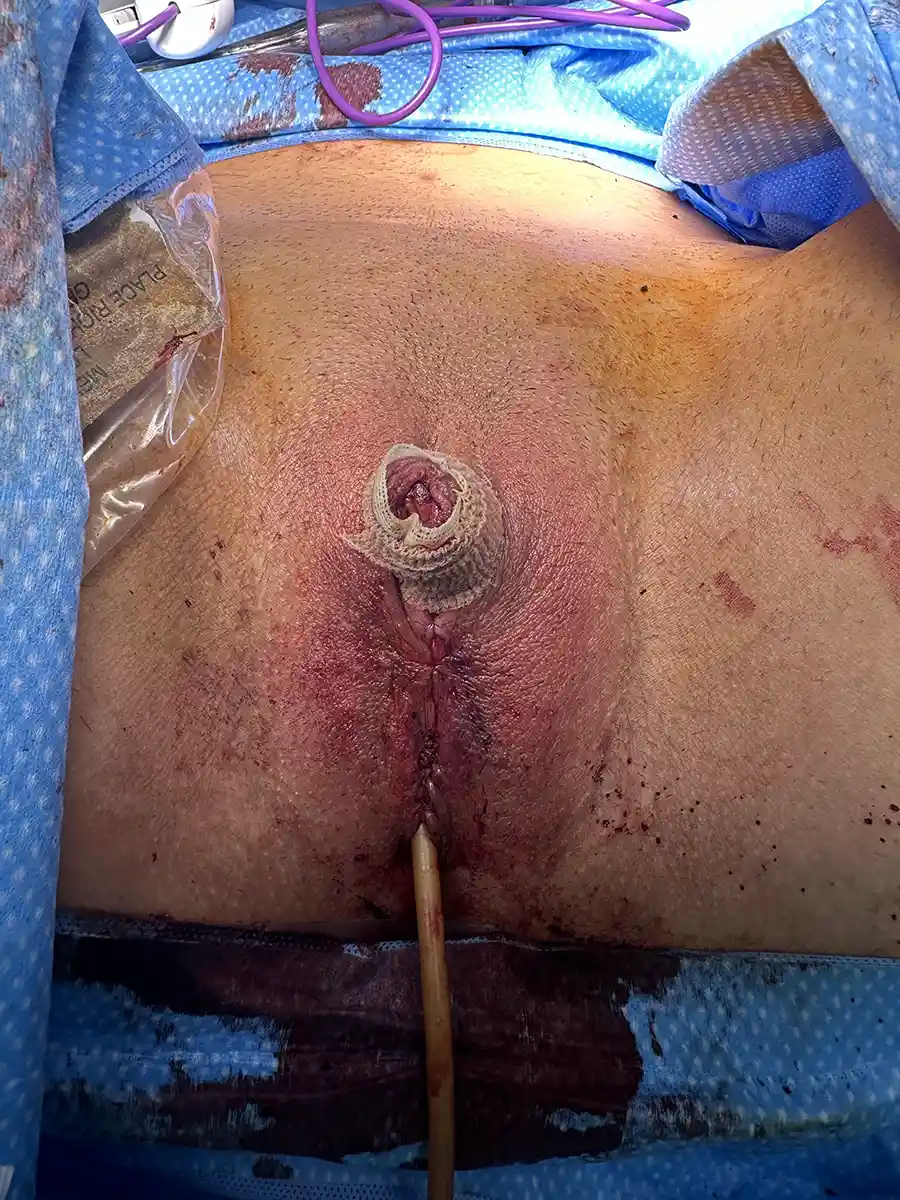
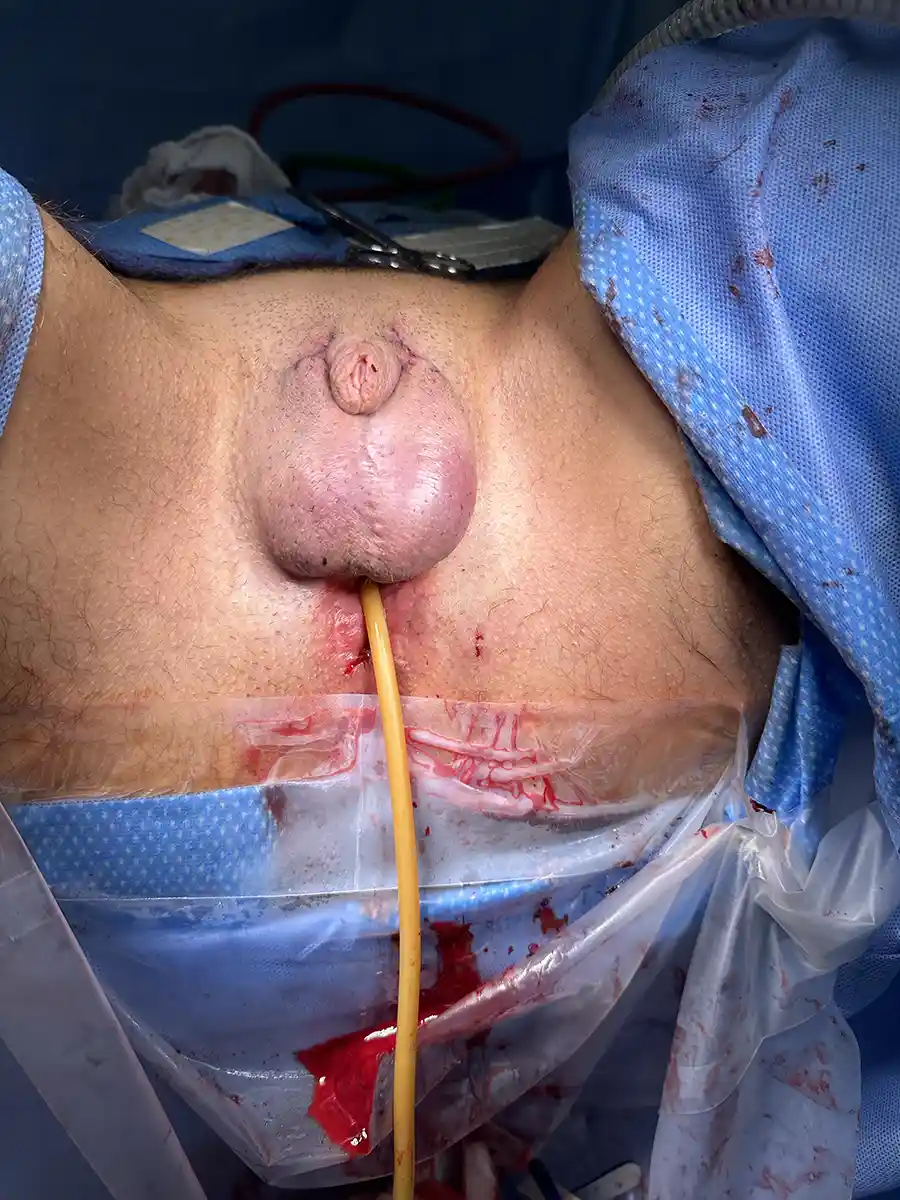
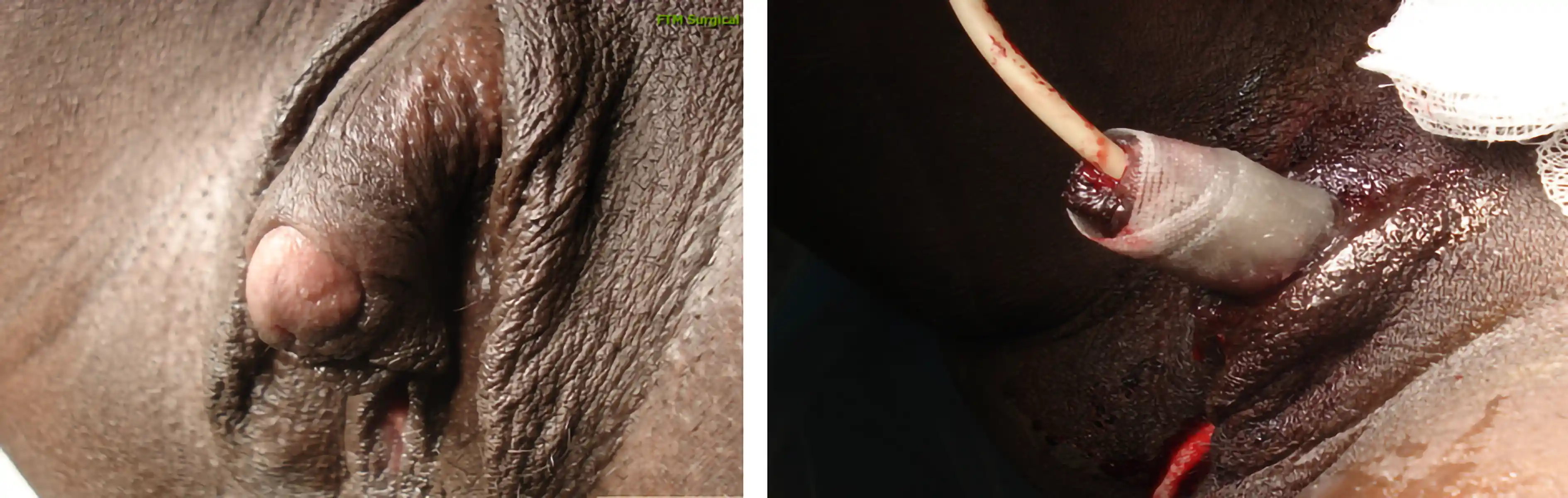
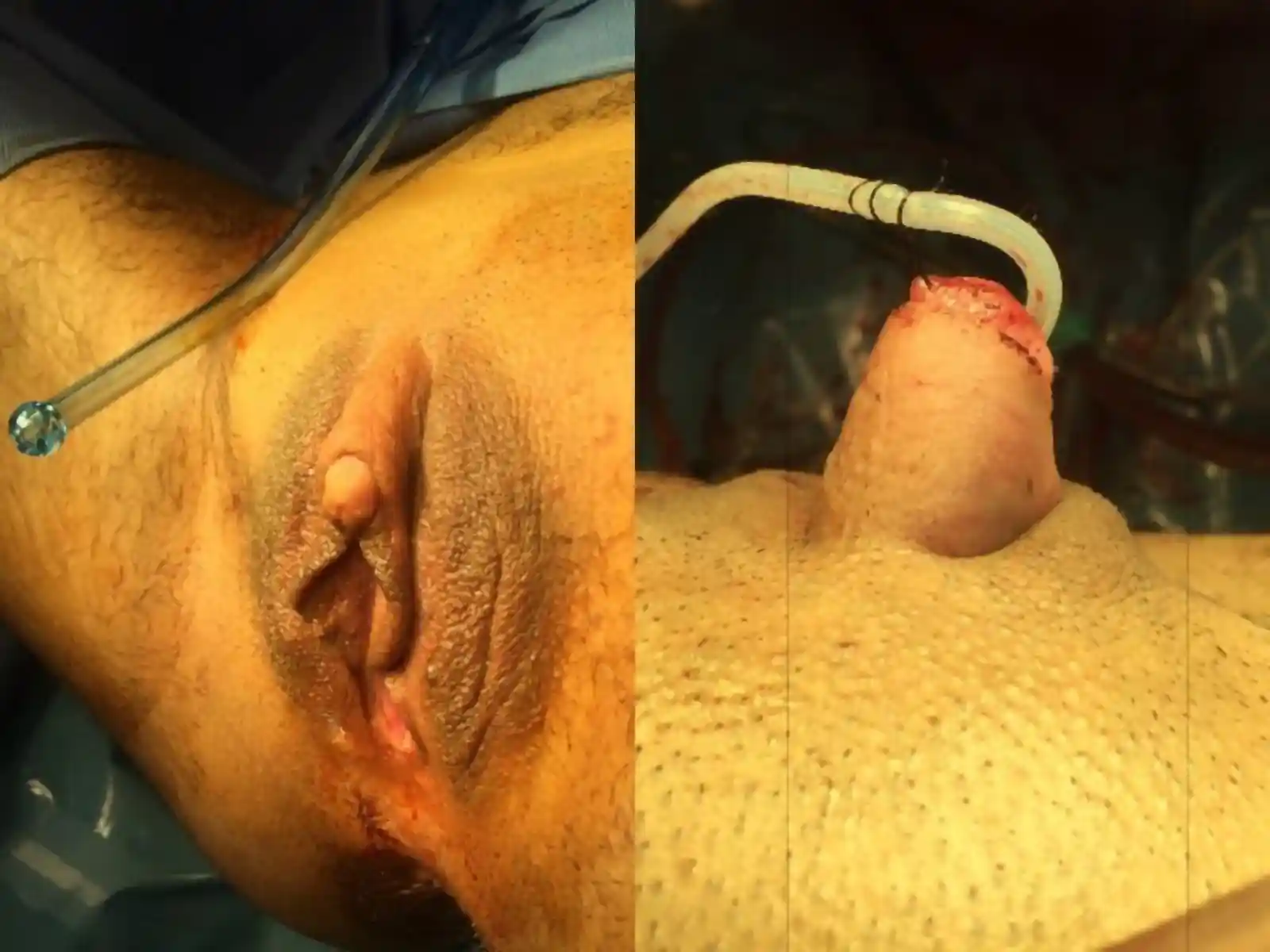
Performed at the same time as metoidioplasty. In this procedure, a skin tube is created from the skin of urethral plate, perineal tissue, and labia minora to extend the urethra with the intended goal of standing to urinate. Often a flap from the vagina is used to cap the lower portion of the urethra (so-called Ring Metoidioplasty). A urinary catheter (e.g. Foley)will be left in place to give the new urethra time to heal before allowing urine to pass through it.
Ideal Candidate:
Someone at a stable weight looking for urethral lengthening with a good amount of tissue to create the urine tube.
Limitations:
It is not always possible to get the urethra to the tip of the penis and therefore, we cannot guarantee that you will be able to stand while urinating. Urethral fistula (an undesirable connection between the urethra and another part of the body) can be a common and difficult problem to resolve in this surgery. Your surgeon will discuss the risks and benefits of this option with you.
A suprapubic catheter will be placed in the lower part of your abdomen directly into your bladder. This will stay in place for 4 weeks while the urethra extension heals. You will also have a catheter in your urethral extension for 1 week. Once this catheter is removed, you will continue to drain urine though the suprapubic catheter. At 4 weeks, we will clamp the suprapubic catheter and will test urinating through the urethra extension. If this is successful, the suprapubic catheter will be removed and allowed to heal.
Further Consideration 1:
For years, surgeons have required vaginectomy as a requisite part of urethral extension. Their argument was that urethral fistula was more common if concurrent or previous vaginectomy was not done. As more patients request non-binary surgical choices, the vagina is often cited as important to retain. It is our opinion that fistula rates are high with urethral extension (30% or more) but that rates are no higher with vaginal conservation as compared to metas with vaginectomy have not been proven.
Further Consideration 2:
All genital procedures whether metoidioplasty or phalloplasty should be considered final. That said, metas with urethral extension can be adapted to later phalloplasty. However, a simple meta is normally not suitable for later urethral extension as part of a phalloplasty procedure because part of the urethral plate is excised in a simple meta.
Further Consideration 3:
Sexual satisfaction with metas seem to exceed that of phalloplasty and increases with time (preliminary data).
III. Preparing for Surgery
Metoidioplasty is a surgery that will limit physical activity for 2-6 weeks, depending on the type of procedure you have. A large part of its success depends on your preparedness. This means being in the best possible physical and mental health before the surgery.
Above all else, it is crucial to have reasonable expectations about what is possible for your body and what your surgeon can realistically accomplish. We recommend you:
- Speak with a mental health professional who has an understanding of gender care to help you navigate this process and exciting period of your life.
- Connect with peers who have been through this surgery for support. Please keep in mind that each person’s surgical plan, experience and result is unique. Information shared on some online forums may not be relevant to your surgery. Due to patient privacy laws, we never comment on another patient’s specific issues or experiences. We are happy to clarify anything related to your individual care.
This guide will help you meet the pre-surgery requirements, prepare for surgery and plan for your recovery. We are here to help ensure that your surgery is successful.
Maximizing Healing
You can expect that surgery will be stressful to your body and that this will require adequate time for healing. In the months and weeks leading up to surgery, maximizing your health—both mental and physical—will aid in achieving a swift recovery.
To optimize healing, we recommend:
- Getting roughly 0.5 gram of protein per weight in lbs a day to maximize healing (e.g. 150lb x 0.5=75g of protein per day).
- Reducing sugar and processed foods.
- Remaining active before having surgery. Keeping up with or adding a workout plan will benefit your overall health and support a speedy recovery. Examples can include adding daily walking, home yoga, or simple home workouts with body weight to your weekly routines.
IV. Planning for Recovery
We understand the importance and urgency of this surgery. We also know your success hinges on being well-prepared. Remember, this is a lifelong investment in your health. Optimal preparation can improve your chances of positive physical and mental health outcomes.
- Home support: In addition to assistance with food, transportation, housework, and running errands, you will require assistance from your caregiver with activities that involve lifting more than 10 lbs. Additionally, you might need support with caring for pets or children.
- Emotional support: You will likely need emotional support, especially for the two weeks while you have limited mobility. Think about what coping strategies you can use during this time.
- Housing
- Utilities
- Groceries
- Medical supplies and medications
- Other bills and expenses
- Make a back-up plan, in case you need more time to heal.
- Find out if you are eligible for Family Medical Leave through your employer. Get your paperwork in early.
- Insurance status
- Moving or loss of housing
- Loss of income and financial concerns
- Different caregiver(s)
- New health condition