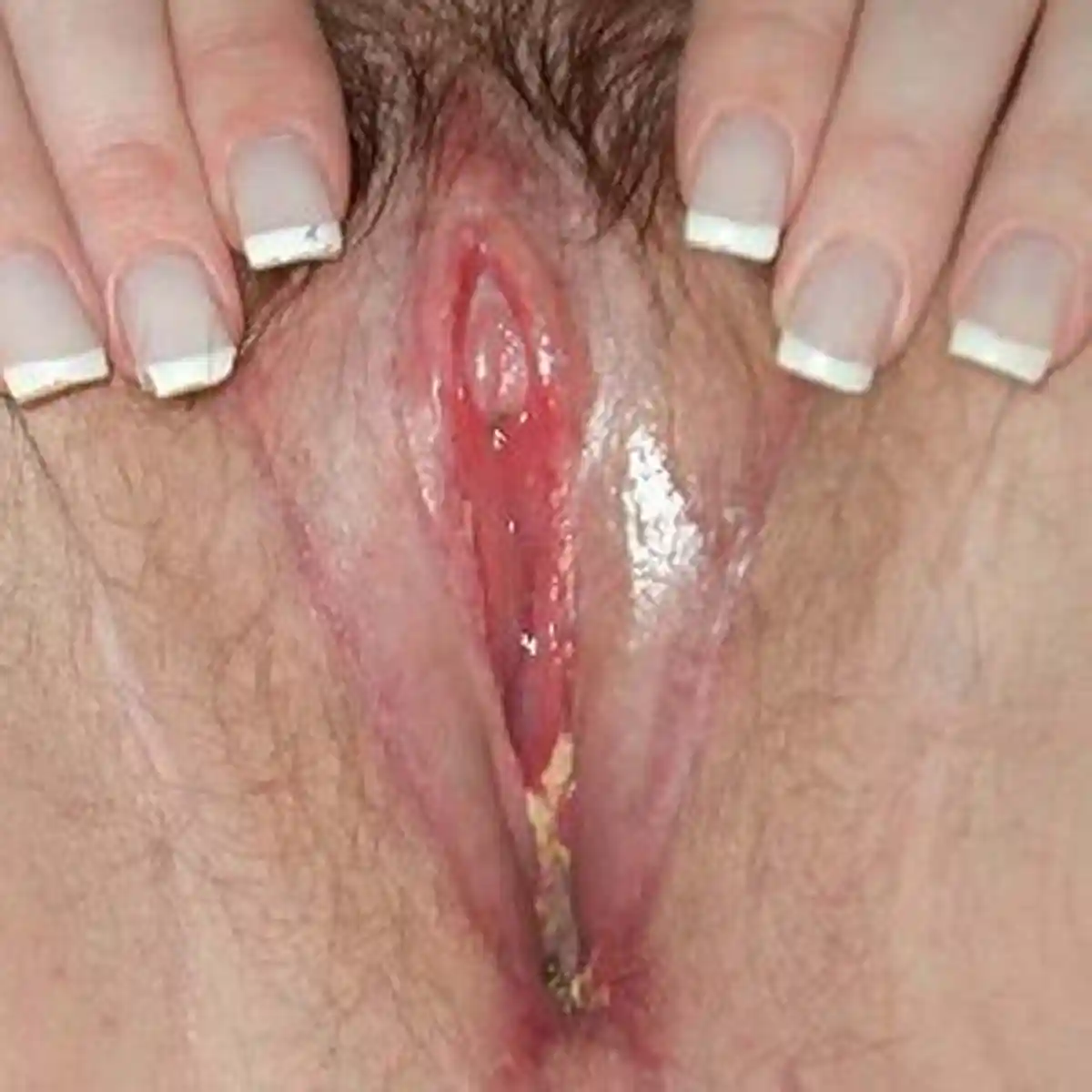
Genital Feminizing
Welcome to Legacy Surgical Partners – we look forward to caring for you! Our priority is to make your surgery process and everything in between as pleasurable, empowering, and accessible as possible. Patients are expected to follow guidelines established by the WPATH Standards of care Version 8. We follow these standards—not as a gatekeeping hurdle—but as minimal guidelines that are useful guideposts that are protective. Though regret for gender affirming surgery is extremely rare, we are medical professionals who are here at your bequest. Surgery is irreversible, which puts the onus of responsibility on both patient and provider.
We're here to help you make essential decisions and know what to expect in surgery planning and recovery. Our team consists of:
- Surgeons
- A physician assistant
- Medical assistants
- Our surgery scheduler
- Office team
- And you 
That’s right, you! We value your input, perspective, and all the work you are doing to prepare for and recover from surgery. We look forward to getting to know you better and learning how we can help you.
I. Genital Feminizing Overview
We understand this surgery is extremely important. It takes a good deal of trust to allow a surgeon to perform this operation. We want to assure you that your trust in our team humbles us, and we take it very seriously.
We’ve created this overview to help you make informed decisions and know what to expect.
What is genital feminizing surgery?
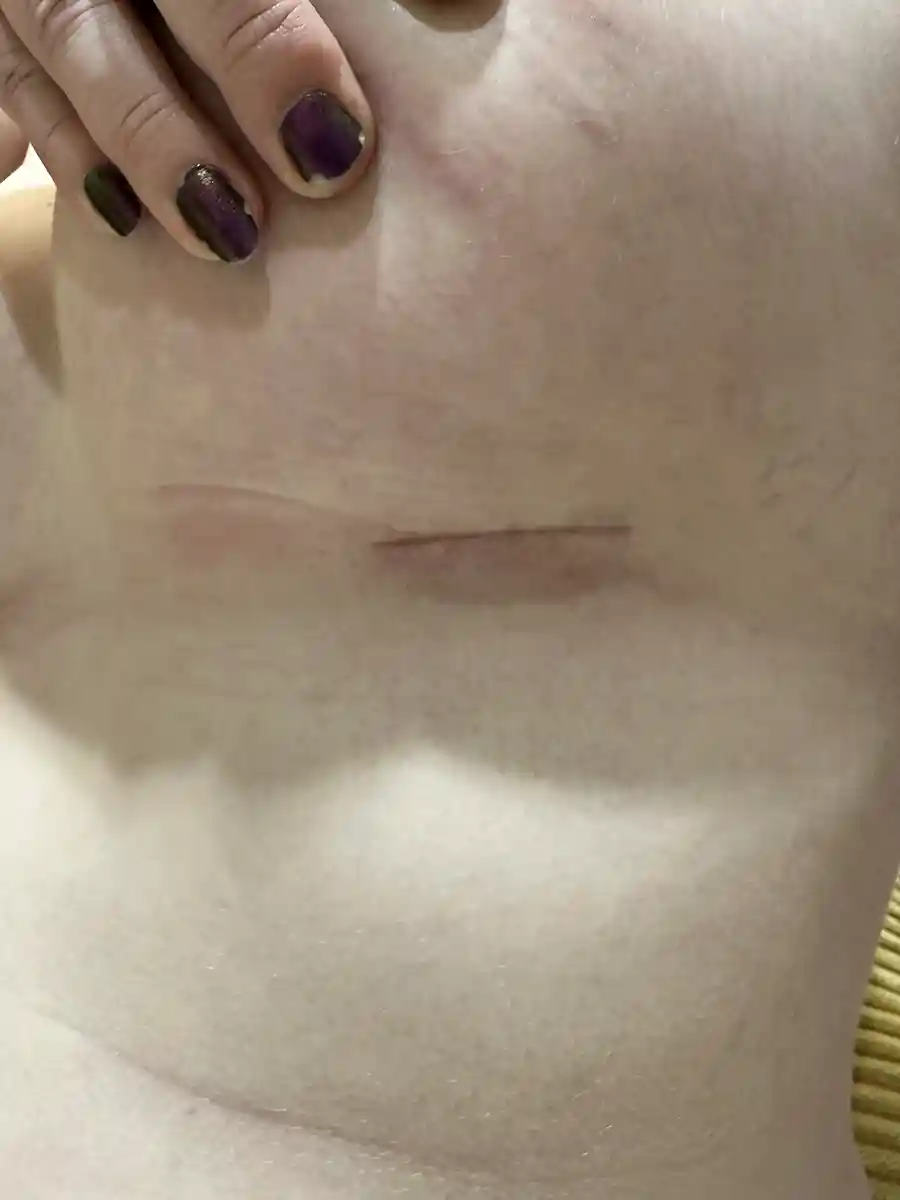
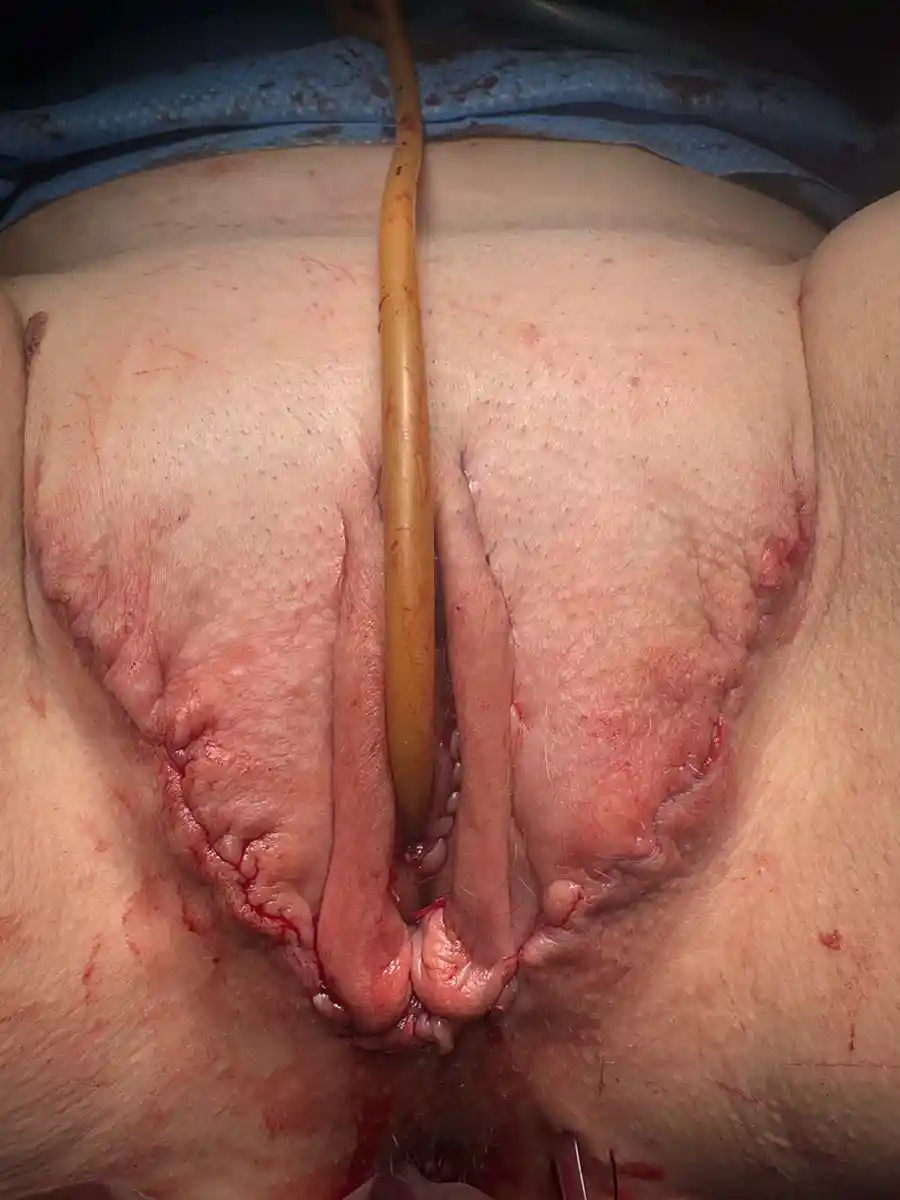
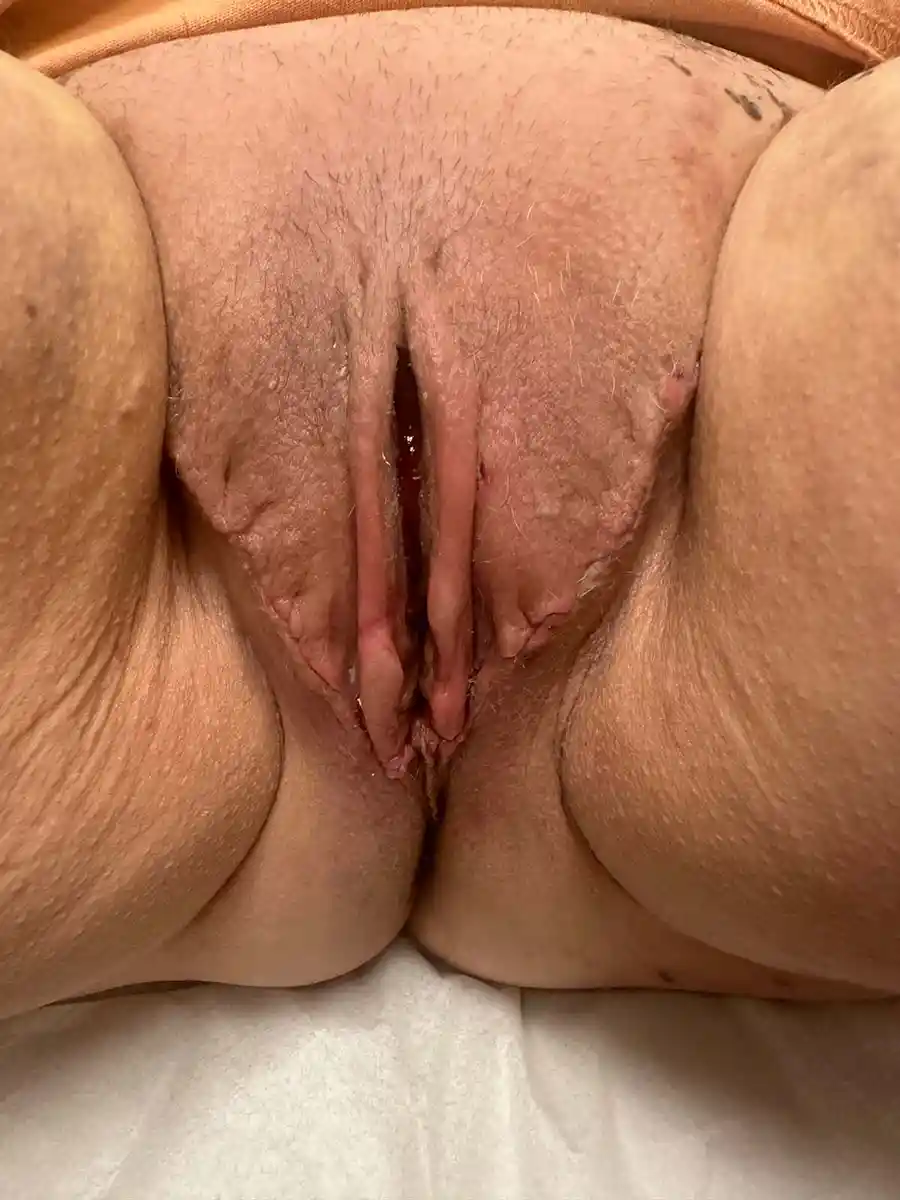
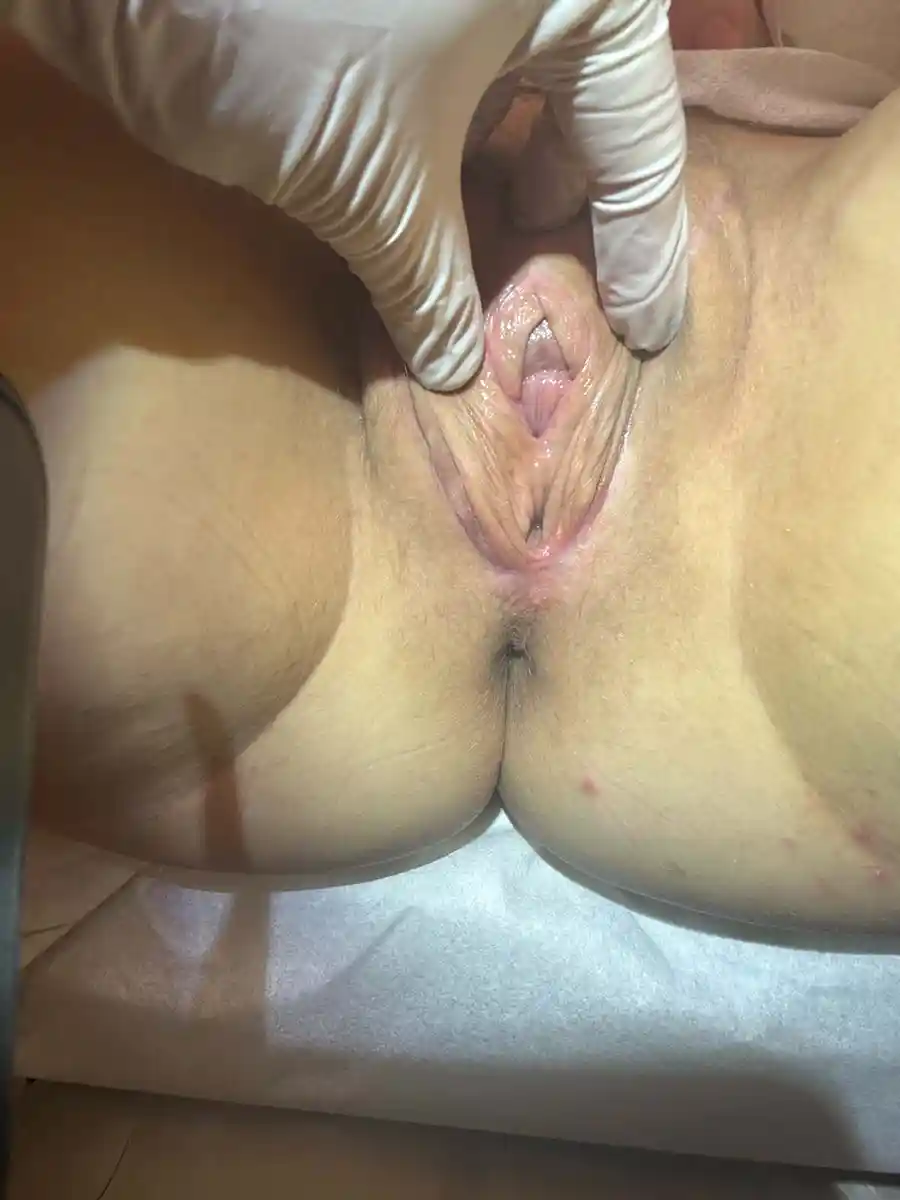
This is an inclusive term that encompasses all the feminizing genital procedures; ie: Vaginoplasty, Vulvoplasty, RoboticPeritoneal Flap Vaginoplasty (RPFV), and non-binary feminizing surgical procedures (Please inquire for alternative options). These procedures are usually a single surgery where tissue is rearranged to create a vulva—or the outside portions of the vagina, clitoris, female-positioned urethra—and if desired, a vaginal canal.
Gender Affirming/Non-Binary Genital Surgery, in ideal circumstances, can enable you to:
- Have a body that more closely aligns with your gender.
- Have a natural-looking vulva with erotic sensations.
- Have a functional vagina with potential for sexual activity including penetration, if desired.
Each patient’s surgery plan and results are different.
II. Before Surgery
Before your first consultation, we encourage you to:
- Consider your goals and priorities for surgery.
- Please write down your questions and bring them with you to your visit.
- Think about whether you want biological children in the future so we can discuss fertility preservation options. There are many resources if you are thinking of preserving sperm.
- You might wish for a support person to come with you. Sometimes there is information discussed with a medical team that is not always remembered. Two heads are often better than one.
Your First Consultation
Your first consultation allows us to learn about your hopes and goals. You may be given a questionnaire to help us meet your needs and measure the results. Your surgeon will review your options and explain the process. You will also get a feel for the office and for the staff. You may also wish to visit Mills-Peninsula Hospital Medical Center at 1501 Trousdale, less than 10 minutes from our office.
Once we understand your goals, we will:
- Evaluate your anatomy, determine the best option based on available tissue
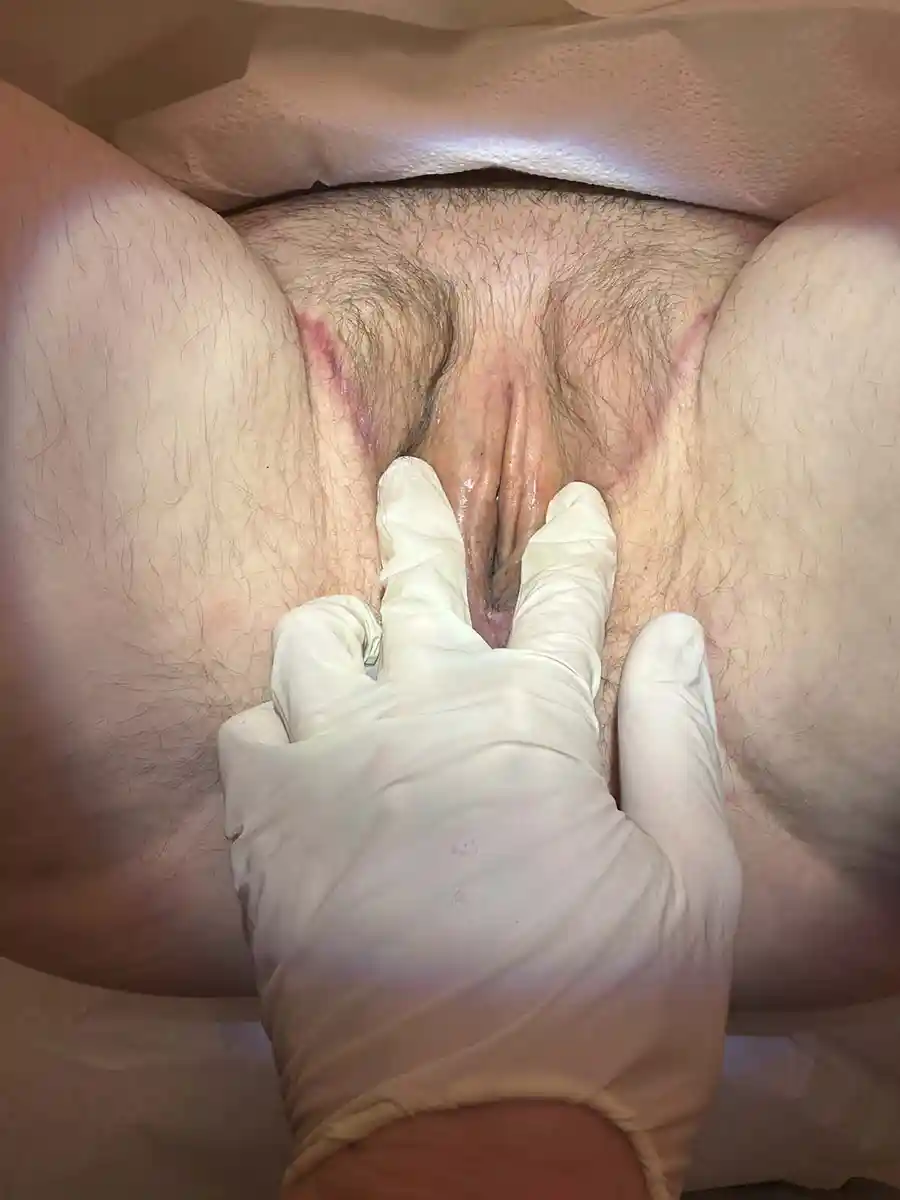
- Look at hair clearance if you have had previous hair removal sessions. Do a brief genital exam and selective physical examination.
- Assess your overall health to see which surgeries can meet your goals. You may be asked to make specific health or lifestyle changes to prepare your body for surgery.
A fair amount of time is spent during the consultation with your surgeon, but you may also meet the other care team members. When team members introduce themselves, they will discuss their role in your care and answer your questions.
Vaginoplasty Options
Each patient’s surgery and results differ as everyone starts with unique anatomy and goals.
Modernized Penile Inversion Vaginoplasty (PIV)
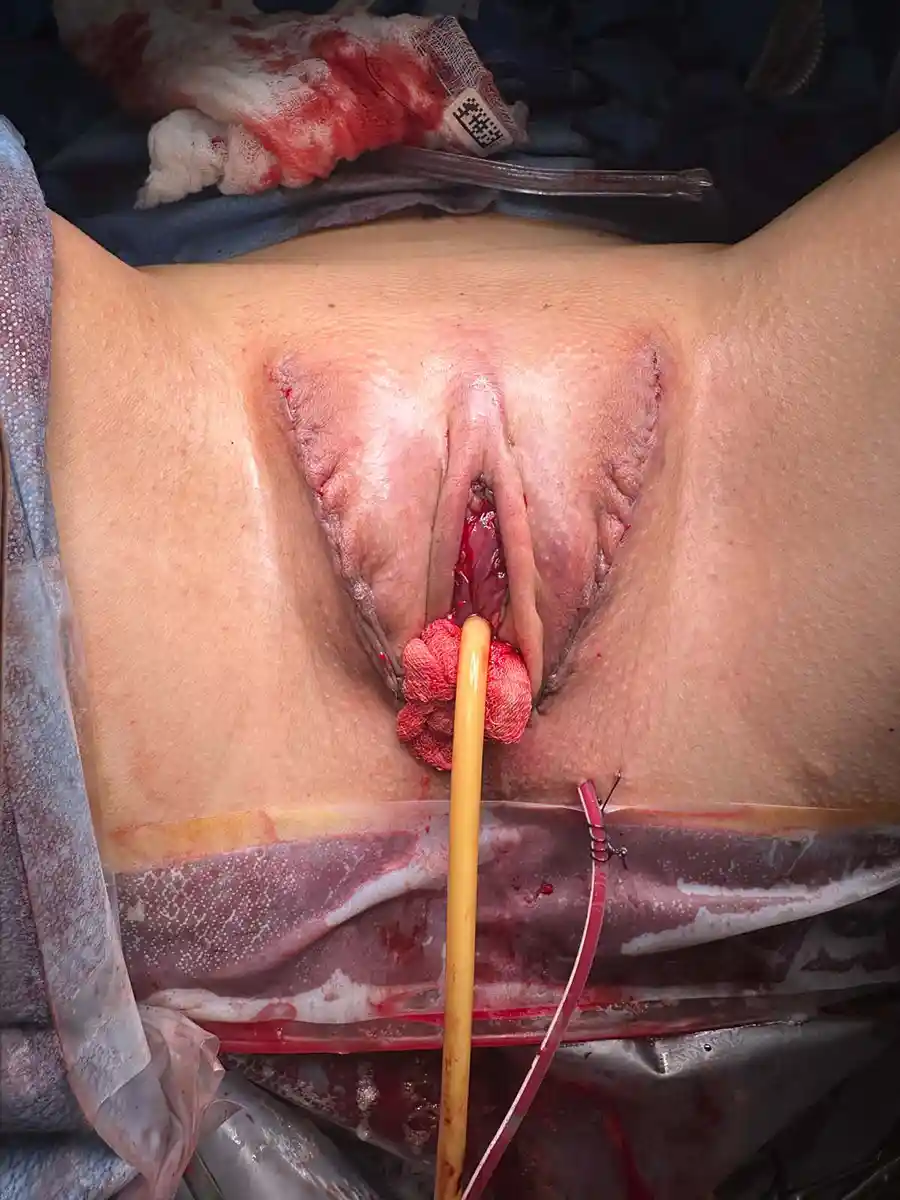
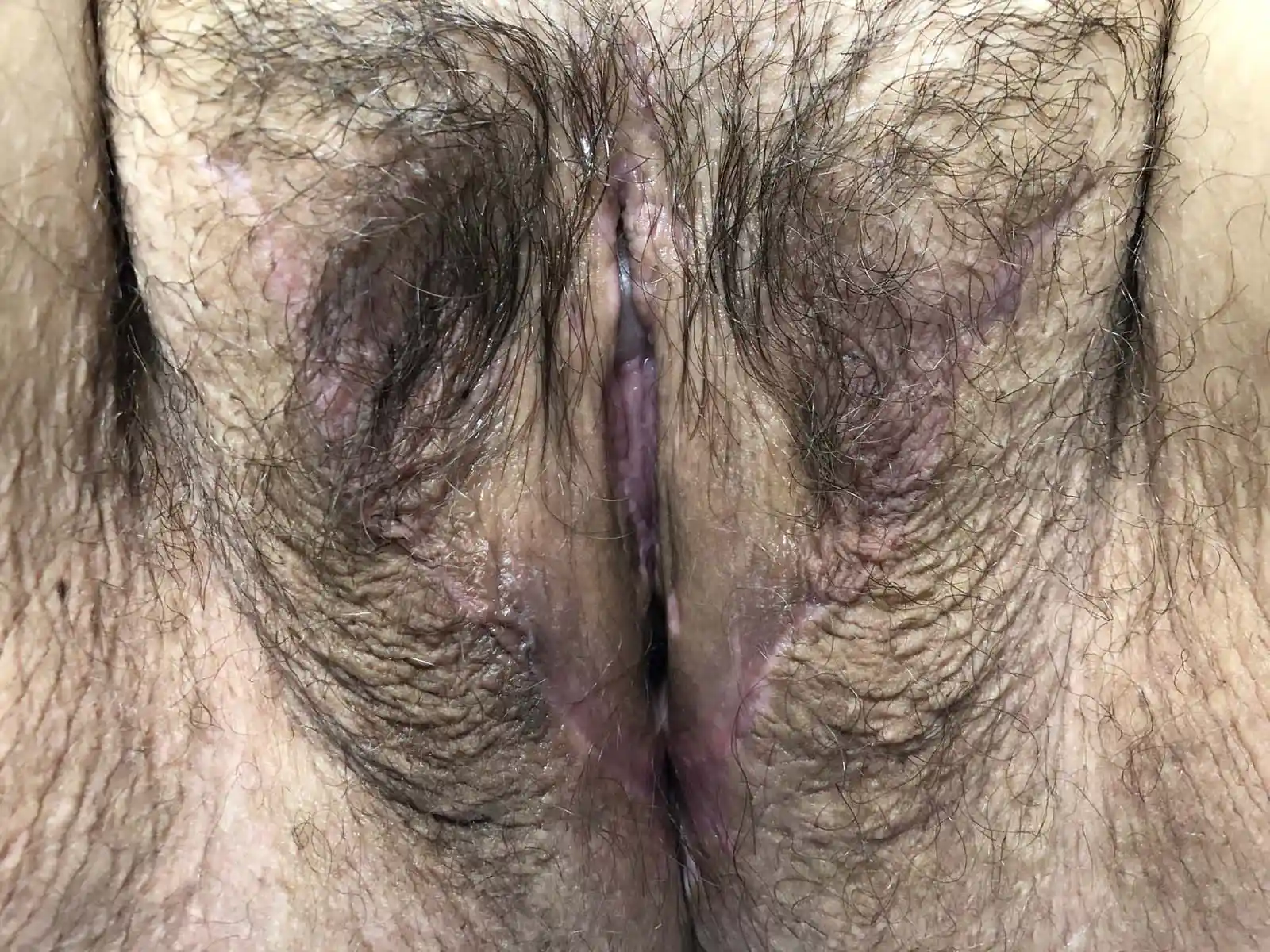
The majority of our patients have enough tissue for this technique. Tissue is rearranged to make full labia majora with defined labia minora and a sensate clitoris with protective hooding along with a vaginal canal with adequate depth and girth for penetrative intercourse, if desired. An area known as the G-Spot/B-spot is also accessible along the front of the neovagina.
Gender Affirming Vaginoplasty is considered a two-step procedure by many surgeons. Under our care, secondary surgeries are necessary less than 10% of the time due to the inclusion of urethral mucosa between the labia minora in combination with surgical precision and symmetry. Revision surgeries are typically cosmetic but can include functional issues such as urination, granulation tissue or scar tissue. Consideration of a second procedure may be discussed while hospitalized but typically best to consider after 6-9 months have passed in order to fully assess the cosmetic outcome though may be planned upon as soon as you feel this might be necessary.
Penile Inversion Vaginoplasty with Additional Graft
With this technique, the external vulva is created the same way as the penile inversion vaginoplasty and the zero depth or minimal depth vulvoplasty. In cases where insufficient tissue is available to line a full-depth vagina, we may discuss options for additional grafts. Options may include using tunica vaginalis — true peritoneum that is available surgically with the removal of the testicles — an additional skin graft, usually from the groin or abdomen, or a skin substitute called an Allograft. Rarely, medical grade Tilapia (fish) skin may be utilized.
Peritoneal Pull Through or Robotic Peritoneal Flap Vaginoplasty (RPFV)
This procedure is generally reserved for patients who have very little tissue available as a result of puberty suppression (blockers) or as a subsequent operation for patients who have lost a considerable amount of depth or who did not have a full vaginal canal created and wish to regain full depth. With this technique, the external vulva is created similarly to the penile inversion vaginoplasty. Available tissue is used to line the more external portion of the vagina. The posterior portion of the canal is lined with a vascular peritoneal graft that is brought down from inside the abdomen by use of robotic surgery. This surgery requires two surgical teams and small surgical sites across the abdomen.
Zero Depth, Minimal Depth, or Vulvoplasty
Though many of our patients choose to have a vaginal canal, this may not be desired by patients who are older, do not wish to perform maintenance dilation of their vagina or who do not hold a need for penetration.
Through this technique, no vaginal canal is created. The vulva is created using similar techniques used in the penile inversion vaginoplasty.
Personal goals for surgery should be carefully weighed against the slightly added risks of full depth vaginoplasty and its implied lifetime commitment to dilation.
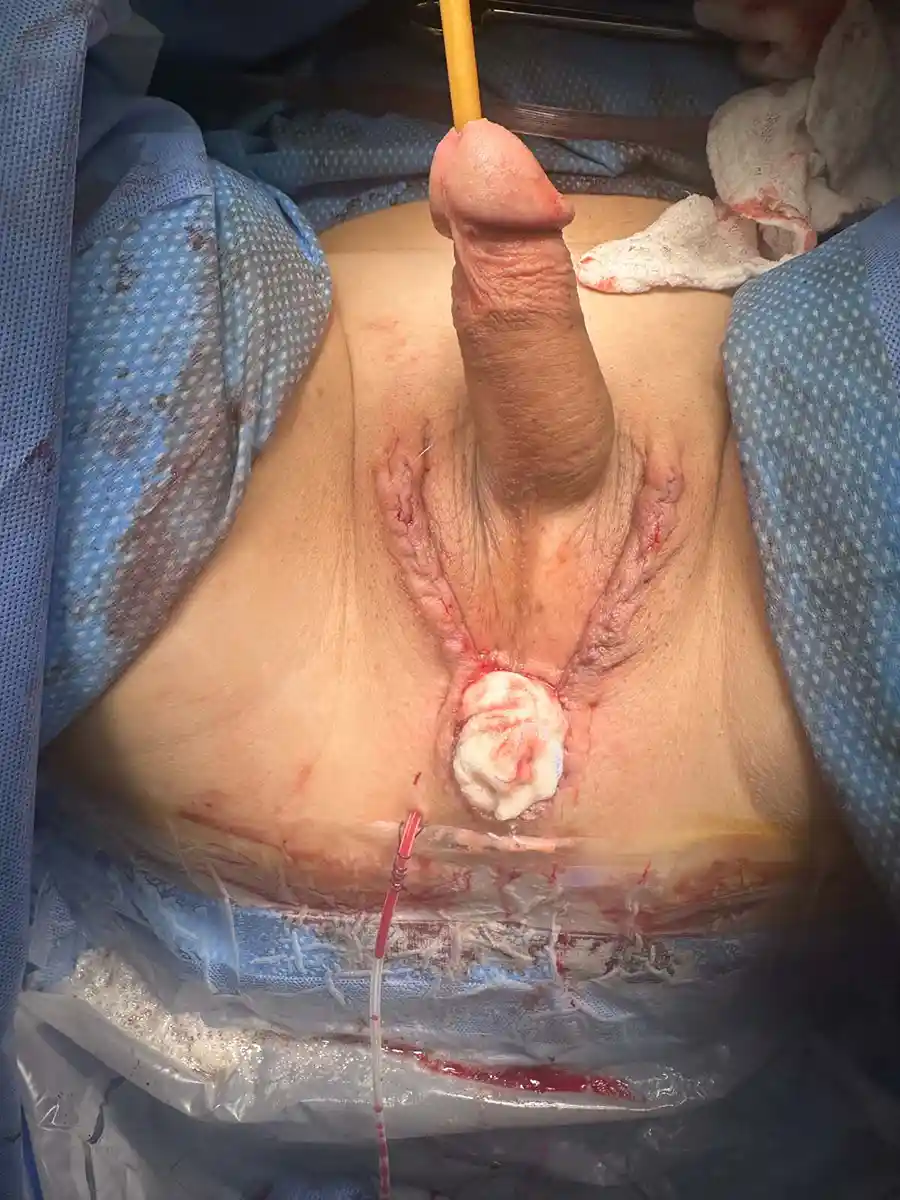
Penile Preserving Vaginoplasty (PPV)
For patients who wish to have a vagina while preserving their penis, PPV may be considered. Please note—following orchiectomy or testicle removal as performed in vaginoplasty, male hormones typically drop, possibly resulting in reduction in libido and reduction in some male sexual characteristics. PPV can be an important choice for a non-binary individual that best fits their personal needs and desires. In this procedure, the penis is preserved and a vaginal canal is created using either available tissue or grafts to give depth to the vaginal canal. This allows for the potential use of the penis as well as a functional vaginal canal.
Nullification or Flat Surgery
For patients that are looking for a flat appearance, nullification is a little-utilized but potential option. In this surgery, the anatomy is rearranged to create a flat genital area, usually with a single vertical midline scar with the urethra at the peroneal or sitting position. The sensate portion of the anatomy can be retrained or buried under the skin, which can allow the ability to maintain orgasm but is not always possible.
Variation Surgery
There can be many variations to the surgeries above. Discuss your options with your surgeon if you are not seeing a surgery above that aligns with your gender identity.
Aesthetic Revisions
Although we aim for a single procedure, about 10% of our patients may desire aesthetic revisions due to variations in anatomy and healing. For minor, in-office procedures and for immediate follow-up, there are no charges. Insurance is typically billed for aesthetic revisions, though we do our best to minimize the necessity of such a secondary procedure. Our practice also commonly does revisions on patients from other practices.
III. Preparing for Surgery
Vaginoplasty is an extraordinarily complex procedure involving multiple steps. Much of its success depends on your preparedness, especially for dilation. This means being in the best possible physical and mental health before the surgery.
Above all else, it is critical to have reasonable expectations about what is possible for your body and what your surgeon can realistically accomplish. We recommend you:
- Speak with a mental health professional who has an understanding of gender care to help navigate this complex process and exciting period of your life.
- Connect with peers who have been through this surgery for support. Please keep in mind that each person’s surgical plan, and experience and result is unique. Information shared on some online forums may not be relevant to your surgery. Due to patient privacy laws, we never comment on another patient’s specific issues or experiences. We are happy to clarify anything related to your individual care.
This guide will help you meet all the pre-surgery requirements, prepare for surgery, and plan for your recovery. We are here to help make sure your surgery is successful.
Maximizing Healing
Although recovery may take up to six months in total, healing is often very rapid with significant reduction in swelling/bruising/discharge just in the first six weeks. You will be dilating during this time 3X daily, which can feel all-consuming. The second six weeks though is considerably easier in most cases as you become comfortable with dilation. After 12 weeks, dilation frequency drops to twice daily. Surgery puts stress on your body, in the months and weeks leading up to surgery, maximizing your health both mental and physical, as this will aid in having a swift recovery. For most, the reality of recovery is easier than imagined.
To maximize healing, we recommend:
- Getting roughly 0.5 gram of protein per weight in lbs a day to maximize healing (eg:150lb x 0.5=75g of protein per day).
- Reducing sugar intake and processed foods.
- Remaining active before having surgery. Keeping up with or adding a workout plan will benefit your overall health and support a speedy recovery. Examples can include adding daily walking, home yoga, or simple home workouts with body weight to your weekly routines.
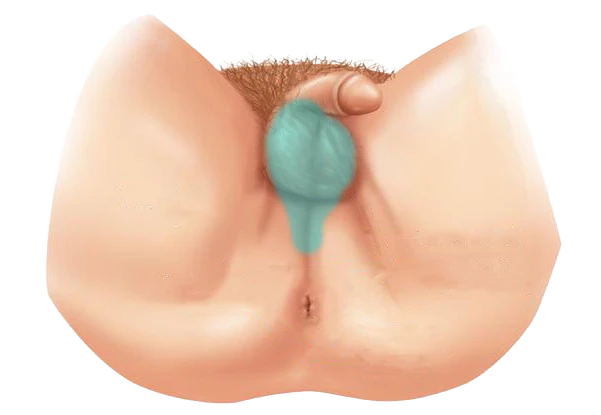
IV. Planning for Recovery
We understand the importance and urgency of this surgery. We also know your success hinges on being well-prepared. Remember, this is a lifelong investment in your health. Optimal preparation can improve your chances of positive physical and mental health outcomes.
- Hospital support: Your caregiver should be with you as much as possible during your hospital stay. Being present during this time will help your caregiver learn from the nurses and surgical team how to care for you once you leave the hospital. Your caregiver must feel comfortable assisting you with genital hygiene care and surgical wound dressing changes. We recommend that your caregiver participate in patient education to learn how to best prepare for their role.
- Home support: You will need your caregiver to help you get to and from the bathroom, shower, complete dressing changes, and help with food, transportation, household chores, and errands. You may also need help with caring for any children or pets.
- Emotional support: You will need a lot of emotional support, especially for the first six weeks of healing. Your primary caregiver will need emotional support as well. Think about what coping strategies you can use during this time.
- Housing
- Utilities
- Groceries
- Medical supplies and medications
- Other bills and expenses
- Make a backup plan in case you need more time to heal.
- Find out if you are eligible for Family Medical Leave through your employer. Get your paperwork in early.
- Hotels: There are several hotels near the hospital. The Sonesta Suites offer Bay Area Reconstructive Healthcare patients and families discounted rates. Please confirm whether your room is accessible by elevator. If not, we recommend staying on the ground level to minimize stair use post-surgery.
- Short-term apartment rentals such as Airbnb or VRBO. Popular locations include Pacifica and Half Moon Bay for their proximity to both the office and the soothing sounds of the Pacific Ocean.
- Insurance status
- Moving or loss of housing
- Loss of income and financial concerns
- Different caregiver(s)
- New health condition